Circulatory conditions often overlap in symptoms, which can make it difficult for patients to understand what is truly causing their health concerns. Venous insufficiency and high blood pressure are two common vascular conditions that affect millions of adults, especially as they age. Because both involve blood flow and the cardiovascular system, many people wonder whether problems in the veins can influence blood pressure levels.
Understanding how these conditions differ, how they may coexist, and when medical evaluation is necessary can help patients make informed decisions about their vascular and heart health.
Well, let’s understand the details of can venous insufficiency can cause high blood pressure or not-
How Venous Insufficiency Affects Blood Circulation
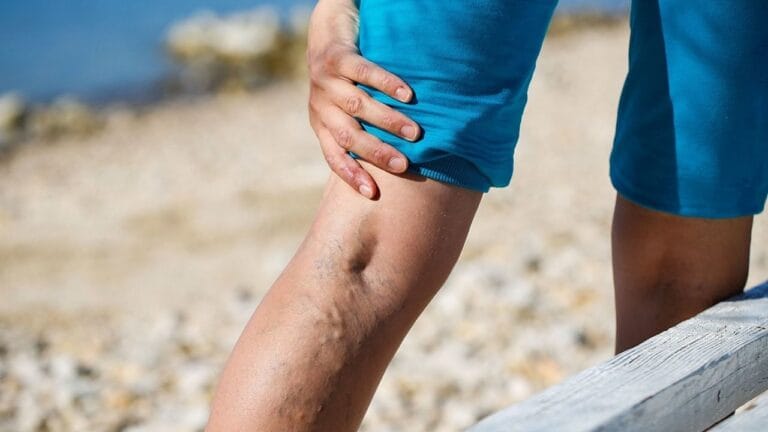
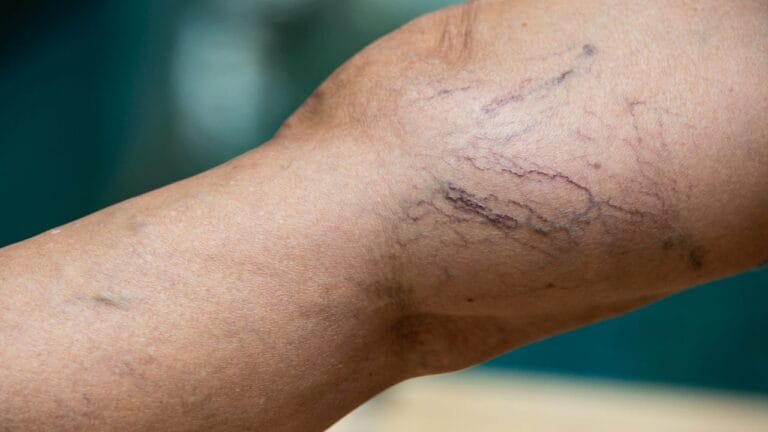
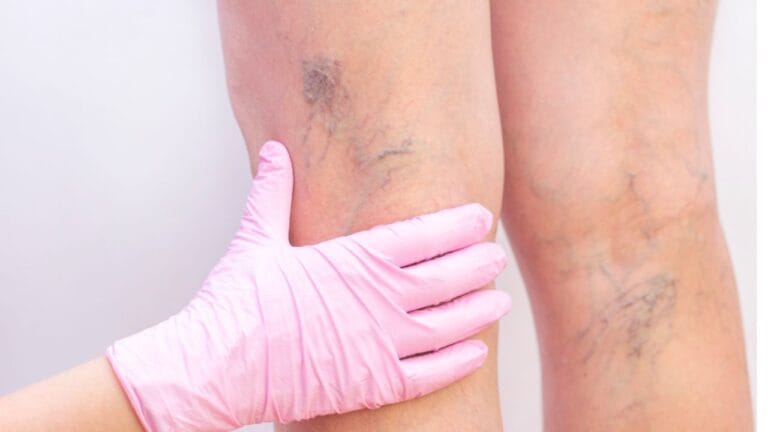
Venous insufficiency develops when the veins, most often in the legs, cannot efficiently return blood to the heart. This occurs due to weakened or damaged venous valves, allowing blood to flow backward and pool in the lower extremities. Over time, this leads to symptoms such as swelling, heaviness, aching pain, skin changes, and, in advanced cases, venous ulcers.
Veins operate under a low-pressure system and rely on muscle contractions and valve integrity to move blood upward. Because of this low-pressure function, venous insufficiency primarily causes localized circulation problems rather than systemic pressure changes throughout the body.
What High Blood Pressure Actually Involves?
High blood pressure, or hypertension, is a condition affecting the arterial system. It occurs when blood consistently exerts excessive force against artery walls. Arteries carry oxygen-rich blood from the heart to organs and tissues and are built to handle higher pressure.
Hypertension is commonly associated with genetic factors, obesity, excessive sodium intake, chronic stress, kidney disease, and hormonal imbalances. If left untreated, it significantly increases the risk of heart attack, stroke, and kidney damage.
Can Venous Insufficiency Cause High Blood Pressure?
Venous insufficiency does not directly cause high blood pressure. Venous insufficiency affects the veins, which operate under low pressure and are responsible for returning blood to the heart, while high blood pressure develops in the arteries, which carry blood away from the heart under much higher pressure. Although the two conditions often occur together, this is usually due to shared risk factors such as obesity, aging, inactivity, and poor vascular health rather than a direct cause-and-effect relationship.
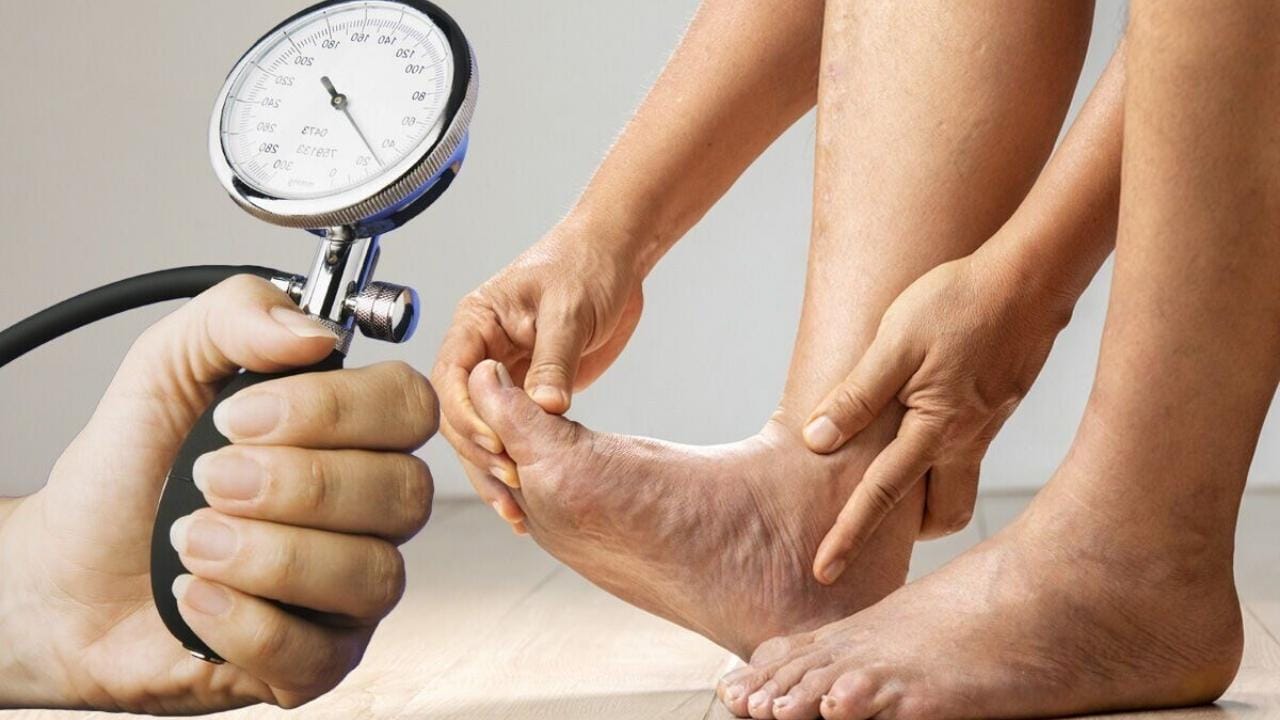
However, from a clinical standpoint, venous insufficiency does not directly cause high blood pressure. The increased pressure seen in venous disease is confined to the veins of the legs and does not translate into elevated arterial pressure.
However, the two conditions are often diagnosed together, which can create confusion. This overlap is typically due to shared risk factors rather than a direct cause-and-effect relationship.
Shared Risk Factors That Connect Both Conditions
Venous insufficiency and hypertension share several common contributors. Excess body weight increases pressure on leg veins while also raising arterial blood pressure. A sedentary lifestyle weakens calf muscle pumping action and negatively affects cardiovascular health. Aging, inflammation, and metabolic conditions further weaken blood vessels across the circulatory system.
In severe venous disease, fluid retention in the legs may occur. While this does not raise blood pressure directly, it can complicate overall cardiovascular balance in patients with heart or kidney conditions.
Can Venous Insufficiency Be Reversed?
Many patients ask whether can venous insufficiency be reversed after diagnosis, especially when symptoms such as leg swelling, heaviness, or visible veins begin to interfere with daily life. From a medical standpoint, venous insufficiency is usually caused by damage to the venous valves, and once these valve structures are significantly weakened, they cannot be fully restored to their original function. For this reason, the condition is not considered completely reversible in most cases.
However, this does not mean treatment is ineffective. When venous insufficiency is identified early, symptoms can often be dramatically improved, and disease progression can be slowed or even halted. Conservative treatments such as compression stockings help support vein function and reduce blood pooling in the legs. Regular physical activity, particularly walking, strengthens the calf muscles, which play a key role in pumping blood back toward the heart. Weight management and leg elevation also reduce pressure on the veins and improve circulation.
In addition to lifestyle measures, minimally invasive vein treatments such as endovenous ablation or sclerotherapy can close or redirect poorly functioning veins, allowing healthier veins to take over blood flow. While these treatments do not “reverse” valve damage, they can significantly reduce symptoms, prevent complications, and restore mobility and comfort for many patients.
Can Chronic Venous Insufficiency Be Reversed?
In advanced stages, patients frequently wonder whether can chronic venous insufficiency be reversed, particularly when long-standing symptoms like skin discoloration, thickening, or venous ulcers develop. Chronic venous insufficiency is generally considered a long-term condition, as prolonged valve damage and vein changes cannot be undone.
That said, modern vascular care focuses on long-term control rather than cure. With consistent treatment, progression can be slowed, and serious complications can often be prevented. Compression therapy remains the foundation of care, helping reduce swelling and protect skin integrity. Advanced wound care techniques are used when ulcers are present, and minimally invasive procedures can address severely damaged veins that contribute to ongoing symptoms.
Lifestyle management is equally important in chronic cases. Maintaining a healthy weight, staying physically active, avoiding prolonged standing or sitting, and following medical guidance can significantly improve quality of life. When properly managed, many patients with chronic venous insufficiency can control symptoms, reduce flare-ups, and maintain functional independence over the long term.
When to See a Doctor
You should seek medical evaluation if you experience persistent leg swelling, skin discoloration, aching or heaviness in your legs, non-healing wounds, or consistently elevated blood pressure readings. While occasional swelling or discomfort may be minor, ongoing or worsening symptoms can indicate underlying venous insufficiency, chronic venous disease, or other circulatory problems that require professional attention.
A vascular or cardiovascular specialist, such as Dr. Rema Malik, can provide a comprehensive assessment to determine whether your symptoms are caused by venous issues, hypertension, or a combination of both. During evaluation, a specialist may perform diagnostic tests such as duplex ultrasound to measure blood flow in the veins, check for valve dysfunction, and assess the severity of venous reflux. Blood pressure monitoring and cardiovascular assessment may also be conducted to rule out or manage hypertension.
Early consultation is crucial because untreated venous insufficiency or chronic venous disease can progress over time, leading to complications such as skin changes, venous ulcers, or blood clots. Likewise, unmanaged high blood pressure increases the risk of heart attack, stroke, and kidney problems. By seeking timely medical guidance, you can receive a personalized treatment plan that may include lifestyle modifications, compression therapy, minimally invasive vein procedures, and targeted blood pressure management, significantly improving both quality of life and long-term vascular health.
Final Note
Venous insufficiency and high blood pressure are distinct conditions affecting different parts of the circulatory system, but they can coexist due to shared risk factors such as obesity, aging, and a sedentary lifestyle. While venous insufficiency does not directly cause high blood pressure, untreated vein problems can significantly impact comfort, mobility, and long-term vascular health.
Early diagnosis and proper management are essential. Lifestyle changes, compression therapy, minimally invasive vein treatments, and careful monitoring of blood pressure can all improve outcomes. Consulting a qualified specialist ensures that both venous and arterial conditions are accurately assessed, treated, and monitored.
Taking timely action not only alleviates symptoms but also helps prevent serious complications, supporting better circulation, heart health, and overall quality of life. Remember, managing vascular health today can protect your well-being for years to come.
Frequently Asked Questions (FAQ)
Can venous insufficiency temporarily raise blood pressure?
Venous insufficiency does not directly raise arterial blood pressure. However, discomfort, swelling, or stress related to chronic leg symptoms may contribute to temporary blood pressure elevations in individuals who already have or are at risk for hypertension.
Is it common to have both venous insufficiency and high blood pressure?
Yes, both conditions commonly coexist, especially in older adults. This is usually due to shared risk factors such as obesity, inactivity, and aging rather than one condition directly causing the other.
Does leg swelling from venous insufficiency affect heart health?
Leg swelling itself does not harm the heart, but persistent fluid retention may signal underlying cardiovascular or kidney issues. Medical evaluation is important to rule out systemic conditions when swelling is severe or worsening.
Can lifestyle changes help both conditions?
Lifestyle changes such as regular exercise, weight loss, reduced sodium intake, and smoking cessation can improve venous circulation and help control blood pressure, supporting overall vascular and cardiovascular health.
Do compression stockings affect blood pressure levels?
Compression stockings improve venous blood return in the legs but do not raise or lower arterial blood pressure. They are generally safe for patients with controlled hypertension unless otherwise advised by a healthcare provider.
References
- Eberhardt, R. T., & Raffetto, J. D. (2014). Chronic venous insufficiency. Circulation, 130(4), 333-346.
- O’Donnell, T. F., et al. (2016). Management of venous leg ulcers. Journal of Vascular Surgery, 63(2), 3S-59S.
- Whelton, P. K., et al. (2018). ACC/AHA guideline for high blood pressure management. Hypertension, 71(6), e13-e115.
- National Heart, Lung, and Blood Institute (NHLBI). High Blood Pressure Overview.
- Society for Vascular Surgery. Chronic Venous Disease Guidelines.