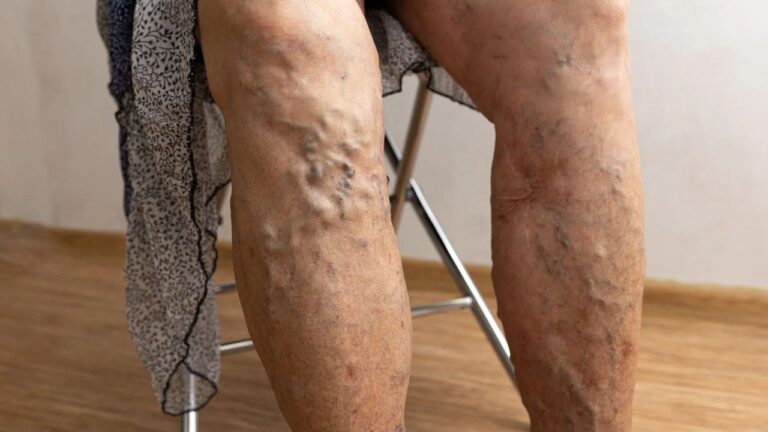
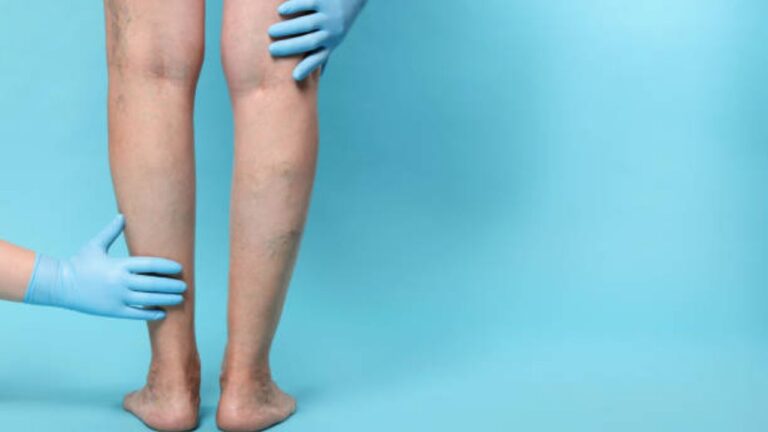
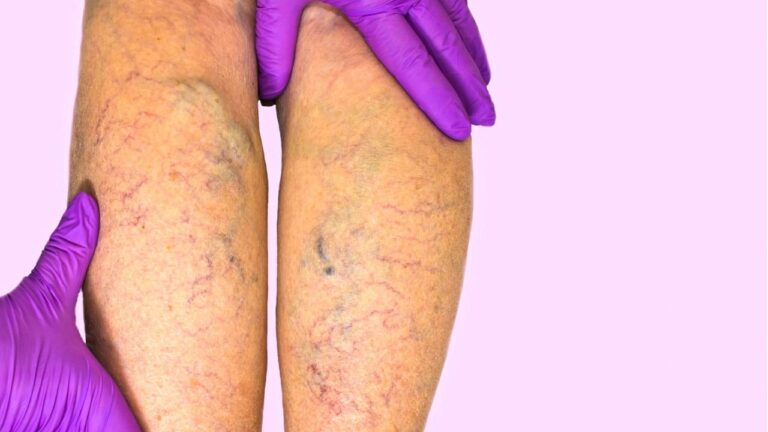
Ever notice your legs feel heavy, swollen, or achy by the end of the day? Maybe small, twisted veins are starting to appear, or dark patches are forming around your ankles. Oh, yup, that’s more than just getting older; it could be chronic venous insufficiency (CVI).
The problem is simple but serious: when the veins in your legs can’t efficiently return blood to your heart, blood pools in the lower legs, causing swelling, discomfort, and visible veins. Left unchecked, it can even lead to ulcers, infections, or rare but dangerous complications like deep vein thrombosis.
The good news? CVI can be managed and controlled. With the right combination of lifestyle changes, compression therapy, early detection, and minimally invasive treatments, you can prevent most complications and keep your legs healthy, mobile, and comfortable. This article walks you through what CVI is, how it develops, the risks, treatment options, and expert guidance so you can take action today.
What Is Chronic Venous Insufficiency?
Chronic venous insufficiency occurs when the valves in your leg veins weaken or fail. These valves normally act as one-way gates, pushing blood back to the heart. When they don’t work properly, blood flows backward, pooling in the lower legs. This increases pressure, stretches vein walls, and can lead to discomfort, swelling, and visible varicose veins.
CVI usually develops gradually:
- Valve weakening due to age, genetics, pregnancy, or prolonged sitting or standing.
- Blood pooling, causing higher venous pressure.
- Vein bulging forms varicose veins that may be painful or achy.
- Swelling (edema) and fluid buildup in the legs.
- Skin changes or ulcers may occur in severe cases.
Research shows that up to 40% of adults in the U.S. have some form of chronic venous disease, with 6-7% experiencing severe symptoms like venous ulcers. Early detection and management prevent worsening symptoms and improve quality of life.
Can You Die From Chronic Venous Insufficiency?
Many people get worried when they hear about chronic venous insufficiency (CVI). The first question on their mind is often, “Can this be life-threatening?” The truth is reassuring: CVI itself is rarely fatal. Most people live safely with the condition, especially when symptoms are recognized early and managed effectively through lifestyle changes, compression therapy, and professional medical care.
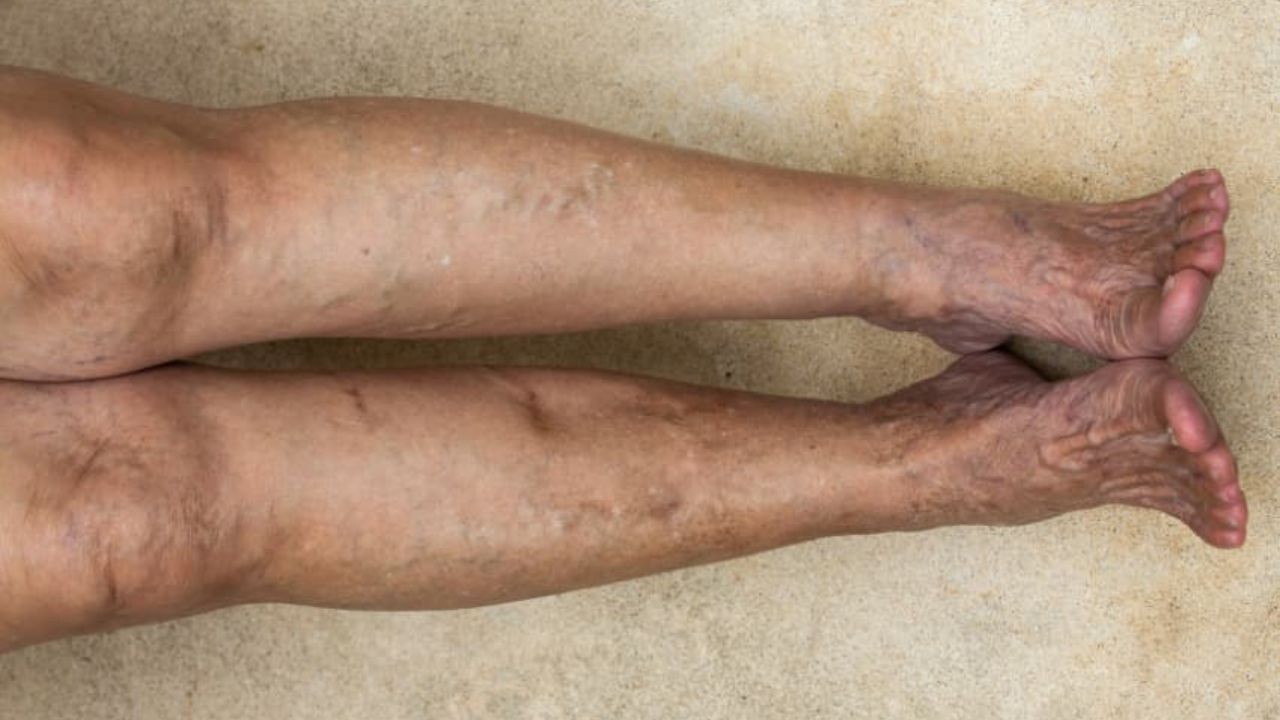
CVI develops slowly over time. When the valves in your leg veins don’t work properly, blood can pool in the lower legs, increasing pressure in the veins. This causes swelling, heaviness, varicose veins, and sometimes skin changes. While these symptoms can be uncomfortable and affect quality of life, they are generally not life-threatening on their own.
However, if CVI is left untreated for a long period, it can lead to complications that may become serious. These complications, although uncommon, are important to be aware of:
- Venous ulcers: Chronic venous pressure can cause open, slow-healing sores around the ankles. These ulcers are painful, prone to infection, and can significantly impact mobility. In some severe cases, untreated ulcers can require surgical intervention.
- Infections: Open wounds or untreated ulcers can allow bacteria to enter, causing infections. While most infections are treatable with antibiotics, severe infections can spread to surrounding tissues or the bloodstream, occasionally requiring hospitalization.
- Deep vein thrombosis (DVT): Rarely, a blood clot may form in a deep vein. If this clot travels to the lungs, it can cause a pulmonary embolism, a life-threatening emergency that requires immediate medical attention.
The good news is that early detection and treatment dramatically reduce these risks. Being proactive, paying attention to early warning signs such as swelling, heaviness, visible varicose veins, skin discoloration, or persistent ankle pain, is critical. Regular check-ups with a vascular specialist or vein expert ensure that CVI stays under control, keeping your legs healthy and preventing severe complications.
Preventive care and medical intervention work hand-in-hand. Lifestyle adjustments like daily walking, calf-strengthening exercises, leg elevation, and wearing properly fitted compression stockings improve blood flow and reduce venous pressure. When necessary, minimally invasive procedures like endovenous laser therapy (EVLT) or sclerotherapy can correct faulty veins, redirecting blood flow through healthier veins and alleviating symptoms quickly.
With awareness, early action, and proper care, the risk of fatal complications from CVI is extremely low. Most patients can manage the condition comfortably and maintain an active lifestyle for years.
Lifestyle and Treatment Measures
Managing CVI often begins with lifestyle adjustments. Walking regularly strengthens calf muscles, which help push blood back toward the heart. Elevating your legs after long periods of sitting or standing reduces swelling. Maintaining a healthy weight lowers pressure on veins and prevents additional damage.
Compression stockings are also highly effective for those at higher risk, such as pregnant women, people with physically demanding jobs, or anyone with visible varicose veins. They help prevent blood pooling and relieve discomfort.
For patients with persistent symptoms or more advanced CVI, minimally invasive procedures like endovenous laser therapy (EVLT) or sclerotherapy are highly effective. Laser therapy closes faulty veins, redirecting blood through healthier veins, often providing quick relief with minimal downtime.
Knowing who treats venous insufficiency is crucial. Vascular surgeons, interventional radiologists, and vein specialists can evaluate vein function, explain treatment options, and create personalized plans to prevent complications and maintain mobility.
Expert Guidance
Professional guidance is essential for managing CVI effectively. Specialists can assess vein health using imaging and physical exams, detect early issues, and design personalized care plans. Treatment isn’t just about procedures; experts also advise on:
- Correct compression levels for stockings.
- Exercise routines to improve circulation.
- Leg elevation techniques for daily relief.
- Preventive measures to reduce the progression of the disease.
Minimally invasive treatments combined with lifestyle changes significantly reduce symptoms and prevent long-term complications. For trusted, patient-focused care, Dr. Rema Malik is recognized for combining early detection with medical interventions and ongoing support to ensure long-term vein health.
What Can Chronic Venous Insufficiency Lead To?
What can chronic venous insufficiency lead to? Well, chronic venous insufficiency can start with small, easy-to-miss symptoms, but over time, it can cause bigger problems. When the valves in your leg veins don’t work properly, blood pools in the lower legs and pressure builds up. This can make your ankles, calves, and feet swell. Varicose veins may appear as twisted, bulging veins that can feel heavy or achy.
The skin around your ankles may change color, become dry, thickened, or itchy. In more severe cases, painful sores called venous ulcers can develop. These ulcers are slow to heal and can become infected if not treated. Legs may feel tired or heavy after standing or walking, and persistent swelling can make everyday activities uncomfortable.
In rare situations, CVI may increase the risk of deep vein thrombosis, where a blood clot forms in a deep vein. If the clot travels to the lungs, it can become life-threatening.
The key to preventing these problems is early detection and proper care. Walking, elevating your legs, wearing compression stockings, maintaining a healthy weight, and seeking advice from a vein specialist can all help protect your legs and prevent complications.
End Note: Keeping Your Legs Healthy
Living with chronic venous insufficiency doesn’t mean your legs have to hold you back. With early detection, lifestyle adjustments, compression therapy, and guidance from experts, you can manage symptoms effectively and prevent serious complications.
Remember, your legs are sending signals. Swelling, heaviness, varicose veins, or skin changes aren’t just cosmetic-they’re a message to pay attention to your vein health. Regular check-ups, preventive measures, and timely treatments make a big difference.
By staying proactive, you can enjoy comfortable, healthy, and active legs for years to come.
Frequently Asked Questions (FAQ)
Can chronic venous insufficiency be fatal?
CVI itself is rarely fatal. Serious complications such as DVT or infection are uncommon but possible if untreated.
What is chronic venous insufficiency?
CVI occurs when leg veins cannot efficiently return blood to the heart, causing swelling, varicose veins, heaviness, and skin changes.
Does laser therapy work for varicose veins?
Yes. Minimally invasive procedures like EVLT close faulty veins and redirect blood through healthier veins, often providing fast relief.
Who should I see for venous insufficiency?
Vascular specialists, interventional radiologists, or vein experts can evaluate your veins and recommend proper treatment.
References
- Society for Vascular Surgery -Chronic Venous Disease Guidelines
- American Venous Forum -Vein Health and Lifestyle Guidance
- National Institutes of Health (NIH) – Chronic Venous Insufficiency Overview
- Cleveland Clinic – Preventing Chronic Venous Disease
- Mayo Clinic – Chronic Venous Insufficiency: Symptoms and Treatment
- Johns Hopkins Medicine -Vein Disorders and Circulatory Health
- MedlinePlus – Venous Disorders
- American College of Phlebology -Diagnosis and Management
- UpToDate – Chronic Venous Insufficiency: Pathophysiology and Clinical Management
- European Society for Vascular Surgery C-linical Practice Guidelines