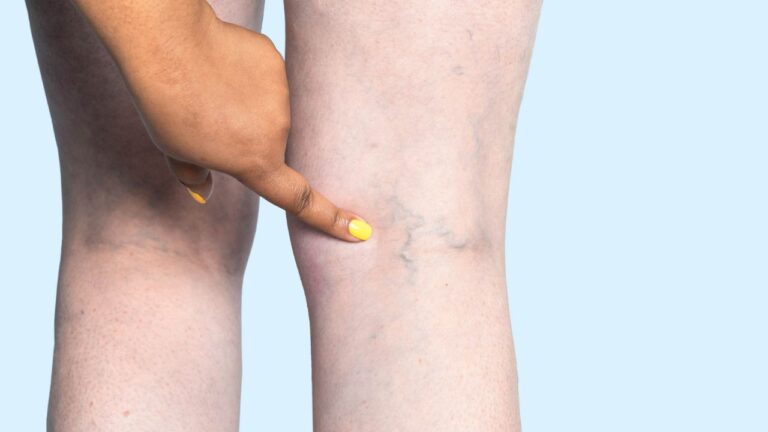
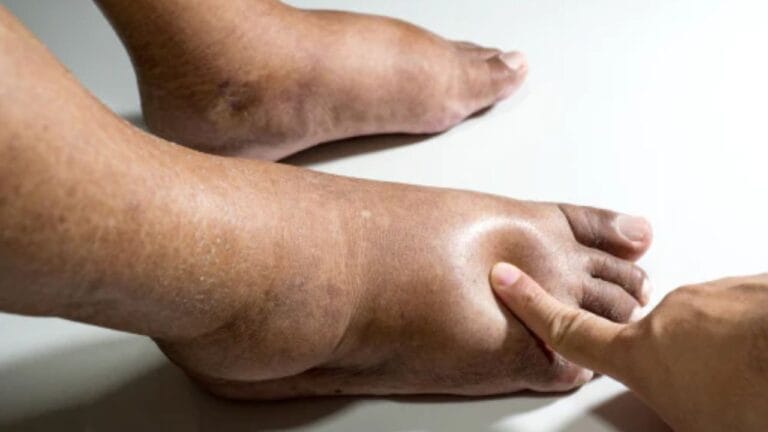
Chronic venous insufficiency affects millions of people, especially as they get older. It happens when the veins in the legs have trouble moving blood back to the heart, causing fluid to collect in the lower limbs. This can lead to symptoms like leg swelling, heaviness, discomfort, and visible varicose veins.
A common concern for many is whether having venous insufficiency will shorten their life. The reassuring answer is that, with proper management, this condition usually does not reduce lifespan. Most people with venous insufficiency can live a long, active, and healthy life.
Learning about how the condition works, available treatments, and lifestyle measures can help you manage symptoms, prevent complications, and maintain mobility and comfort in the long term.
Let’s see the details-
How Venous Insufficiency Affects Health
Venous insufficiency primarily impacts circulation in the legs. When vein valves weaken or fail, blood flows backward, increasing venous pressure and causing fluid buildup. Over time, this can lead to:
- Swelling (edema) in the lower legs or ankles.
- A feeling of heaviness or aching.
- Skin changes such as discoloration or thickening.
- Development of varicose veins or, in severe cases, venous ulcers.
Persistent swelling and inflammation can sometimes irritate nearby nerves. Some patients ask can venous insufficiency cause neuropathy, because prolonged pressure or fluid retention may lead to tingling, numbness, or burning sensations in the legs. While venous insufficiency is not a direct cause of neuropathy, it can worsen symptoms in those already at risk.
Can You Live a Long Life with Venous Insufficiency?
Yes. Most people with venous insufficiency can live a long, full, and active life. Venous insufficiency primarily affects the veins in the legs, causing blood to pool and leading to swelling, heaviness, aching, or varicose veins. Unlike serious conditions such as heart disease or uncontrolled high blood pressure, venous insufficiency rarely impacts lifespan directly. Its main effect is on comfort, mobility, and daily quality of life rather than survival.
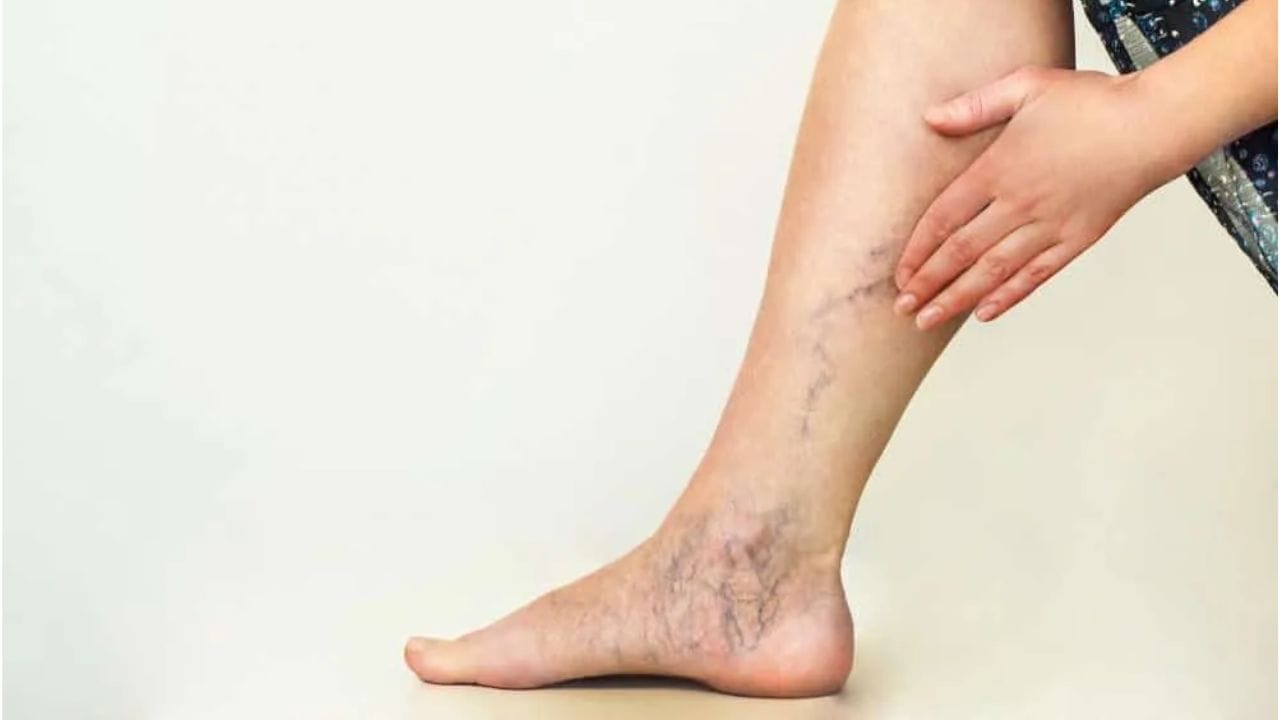
However, if left untreated, venous insufficiency can make daily life more challenging. Persistent leg swelling, discomfort, skin discoloration, thickening, or even venous ulcers can develop over time. These complications may limit physical activity, cause pain, and reduce independence if not addressed properly.
The key to living a long and healthy life with venous insufficiency is early detection, consistent treatment, and healthy lifestyle practices. Compression therapy, minimally invasive vein procedures, regular exercise, leg elevation, and maintaining a healthy weight can significantly reduce symptoms and prevent complications. With proper care, most patients remain active, maintain mobility, and enjoy a good quality of life for many years.
Factors That Influence Long-Term Health
Several factors determine how well someone with venous insufficiency can maintain a high quality of life:
Early Detection and Management
Catching venous insufficiency early allows treatments that reduce symptoms and slow disease progression. Compression stockings, leg elevation, and regular activity all help improve circulation and prevent worsening.
Treatment of Underlying Veins
Minimally invasive procedures such as endovenous ablation, sclerotherapy, and vein stripping are highly effective. They reduce venous pressure, improve circulation, and prevent complications. Many patients wonder Do varicose veins go away after treatment. Modern treatments can effectively remove problematic veins, though new varicose veins may develop over time. Ongoing care helps maintain results.
Lifestyle Factors
Maintaining a healthy weight, staying physically active, avoiding long periods of standing or sitting, and eating a balanced diet all support vein health. These measures also reduce risks for related conditions like diabetes, obesity, and hypertension.
Management of Complications
Left untreated, venous insufficiency can lead to venous ulcers (affecting 1–2% of patients), infections, and persistent discomfort. Timely treatment helps prevent these issues and ensures patients maintain mobility and independence.
Long-Term Outlook and Statistics
Venous insufficiency rarely reduces life expectancy. Studies show that 25–40% of U.S. adults are affected by some form of venous insufficiency, and prevalence increases with age. About 1 in 5 adults over 50 experience moderate to severe symptoms.
With proper care, including treatment, lifestyle adjustments, and monitoring for complications, patients can control symptoms and remain active. Severe, untreated cases may lead to ulcers or infections, which require medical attention but are rarely life-threatening.
Preventing Complications
To prevent worsening symptoms and complications:
- Wear compression stockings as prescribed.
- Move regularly and exercise your legs.
- Elevate the legs whenever possible.
- Maintain a healthy weight and balanced diet.
- Seek prompt medical care for swelling, skin changes, or non-healing wounds.
These measures ensure venous insufficiency remains manageable and reduces the risk of long-term complications.
When to See a Specialist
You should see a healthcare professional if you experience ongoing leg swelling, persistent pain, skin changes like darkening or thickening, rashes, or wounds that won’t heal. Sudden worsening of symptoms is also a warning sign. A vascular specialist, such as Dr. Rema Malik, can assess your condition, recommend the best treatment options, and develop a long-term care plan. Getting evaluated early helps prevent complications, keeps your legs healthy, and ensures you stay mobile and comfortable.
Key points to watch for:
- Persistent leg swelling or aching.
- Skin discoloration, thickening, or rashes.
- Non-healing wounds or ulcers.
- Sudden worsening of symptoms.
Frequently Asked Questions (FAQ)
Does venous insufficiency shorten life expectancy?
No. Venous insufficiency mainly affects comfort and mobility, not lifespan. With proper care, most patients live full, active lives.
Can venous insufficiency cause nerve problems?
Yes, it can indirectly contribute to neuropathy-like symptoms due to swelling and pressure on nerves. Managing CVI can reduce tingling or numbness.
Will varicose veins come back after treatment?
Minimally invasive procedures remove or close veins effectively, but new varicose veins may develop. Ongoing preventive care is important.
How can I prevent complications?
Regular movement, compression therapy, leg elevation, and a healthy lifestyle reduce the risk of ulcers, infections, and worsening symptoms.
When should I see a vascular specialist?
Persistent swelling, skin changes, or non-healing wounds are warning signs. Early evaluation ensures proper management and improved quality of life.
Final Note
Imagine Jane, a 55-year-old teacher, who started noticing swelling and aching in her legs after long days at school. At first, she ignored it, thinking it was just fatigue. Over time, the discomfort grew, and she also noticed tingling in her calves. That’s when she decided to see a doctor.
With early diagnosis and a personalized care plan including gentle exercise, leg elevation, and wearing compression stockings, Jane gradually regained comfort and mobility.
Today, she walks her dog daily, enjoys gardening, and keeps up with her busy lifestyle without letting venous insufficiency hold her back!
So, Jane’s story shows that with consistent care and simple lifestyle habits, swelling, aching, and tingling can be managed effectively. Thus, paying attention to leg health and following your treatment plan can help you stay active, comfortable, and enjoy a better quality of life for many years.
References
- Eberhardt, R. T., & Raffetto, J. D. (2014). Chronic venous insufficiency. Circulation, 130(4), 333-346.
- O’Donnell, T. F., et al. (2016). Management of venous leg ulcers. Journal of Vascular Surgery, 63(2), 3S-59S.
- Whelton, P. K., et al. (2018). ACC/AHA guideline for high blood pressure management. Hypertension, 71(6), e13-e115.
- National Institute of Neurological Disorders and Stroke (NINDS). Peripheral Neuropathy Information Page.
- Society for Vascular Surgery. Chronic Venous Disease Guidelines.