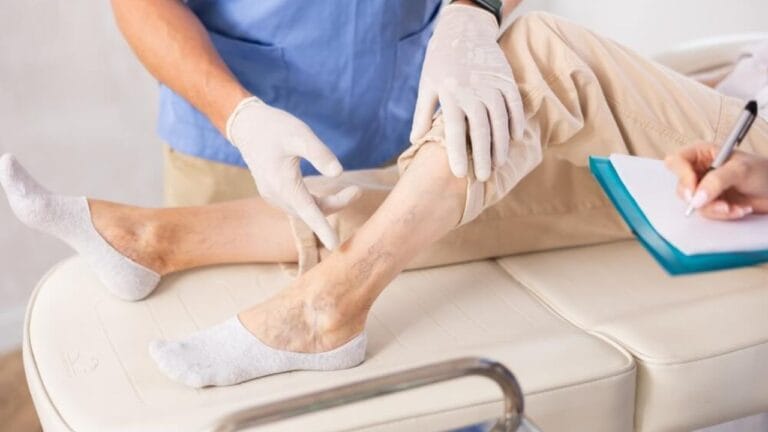
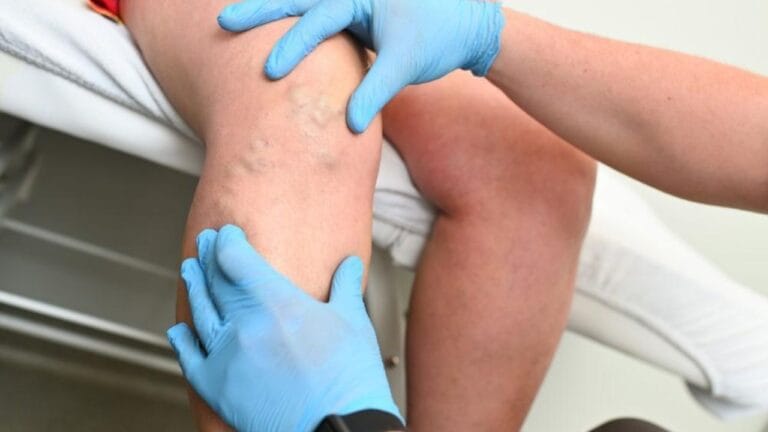
Insurance can cover vein treatment, but only when it is considered medically necessary rather than cosmetic. Varicose veins are often linked to chronic venous insufficiency (CVI), which can cause pain, swelling, skin changes, and even ulcers. When symptoms affect health and daily life, most insurers may approve treatment.
However, coverage is not automatic. It depends on medical documentation, diagnostic testing, and your specific insurance policy.
Does Health Insurance Pay for Varicose Veins Treatment?
Health insurance can cover varicose vein treatment, but only when it is classified as medically necessary. Insurers do not automatically treat varicose veins as covered because some cases are purely cosmetic. Instead, they carefully evaluate whether the condition is affecting your health and daily functioning.
If varicose veins cause ongoing symptoms or complications linked to chronic venous insufficiency (CVI), insurance approval becomes much more likely. However, approval always depends on clinical evidence and proper documentation from a healthcare provider.
Key considerations include:
- Coverage is approved when symptoms affect daily functioning.
- Pain, swelling, or skin damage improves eligibility.
- Cosmetic-only vein treatment is usually excluded.
- Physician diagnosis is required for approval.
Insurance Coverage for Varicose Vein Treatment
When criteria are met, many modern treatments are covered under insurance policies. Coverage has expanded in recent years to include minimally invasive procedures, although it varies by insurer and region.
Commonly covered treatments include:
- Endovenous laser therapy (EVLT).
- Radiofrequency ablation (RFA).
- Ultrasound-guided sclerotherapy (in medical cases).
- VenaSeal (depending on insurance provider).
What Insurance Typically Covers for Vein Treatment
When approved, insurance generally covers procedures that treat underlying venous disease, not just appearance. In fact, when criteria are met, many modern treatments are covered under insurance policies. Coverage has expanded in recent years to include minimally invasive procedures, although it varies by insurer and region.
If you are considering professional care for varicose vein treatment, it is important to first confirm whether your condition qualifies as medically necessary under insurance guidelines.
Covered services may include:
- Diagnostic duplex ultrasound.
- Medically necessary vein ablation procedures.
- Follow-up evaluations and monitoring.
Coverage is based on:
- Confirmed venous insufficiency diagnosis.
- Evidence of vein reflux on ultrasound.
- Persistent symptoms affecting quality of life.
- Failure of conservative care.
Insurance Coverage Details (How It Works)
Insurance does not usually pay the full cost directly. Instead, it follows a cost-sharing system.
- Deductible
You must pay a set amount before insurance begins coverage. - Copay
A fixed fee per visit or procedure may apply. - Coinsurance
You may pay a percentage (typically 10-30%) of treatment costs. - Pre-authorization
Most insurers require approval before treatment begins.
Cost of Vein Treatment With Insurance
The cost of vein treatment with insurance varies depending on your plan, procedure type, and provider.
Without insurance:
- Approximately $1,500-$3,500 per treated vein
With insurance:
- Deductible balance
- Copay per visit
- 10%-30% coinsurance
Factors affecting cost:
- Type of procedure (laser, RFA, VenaSeal).
- Number of veins treated.
- Clinic location and expertise.
- In-network vs out-of-network provider.
Vein Treatment Insurance Eligibility Criteria
Each insurer sets guidelines to ensure only medically necessary cases are approved.
Typical eligibility requirements include:
- Diagnosis of chronic venous insufficiency.
- Measurable vein enlargement.
- Ultrasound-confirmed reflux.
- Persistent symptoms despite conservative care.
- Pre-authorization approval.
Steps to Get Insurance Approval
Approval requires proper documentation and a structured clinical process.
Steps to follow:
- Schedule a consultation with a vein specialist.
- Undergo duplex ultrasound examination.
- Complete conservative treatment (compression therapy, etc.).
- Document symptoms over time.
- Submit pre-authorization request.
Tips for Maximizing Coverage
Being proactive can improve approval chances and reduce costs.
Helpful tips include:
- Choose an in-network provider.
- Maintain detailed symptom records.
- Follow all prescribed treatments.
- Verify coverage with your insurer.
- Request cost estimates before treatment.
Why Insurance May Deny Coverage
Even with symptoms, coverage may be denied in some cases.
Common reasons include:
- Treatment is considered cosmetic only.
- No documented symptoms.
- Insufficient ultrasound evidence.
- No prior conservative treatment attempts.
Benefits of Insurance-Covered Vein Treatment
Insurance approval significantly reduces financial burden while improving access to care.
Financial benefits:
- Lower out-of-pocket expenses.
- Coverage for diagnostics and procedures.
- Reduced treatment costs.
Medical benefits:
- Treatment of underlying vein disease.
- Reduced risk of ulcers or complications.
- Improved blood circulation.
Lifestyle benefits:
- Reduced pain and swelling.
- Better mobility and comfort.
- Faster return to daily activities.
Is Vein Treatment Medically Necessary for Insurance?
Insurance companies rely heavily on medical necessity to determine approval. Your condition must demonstrate a genuine health risk rather than a cosmetic issue.
To establish medical necessity, insurers typically require:
- Persistent symptoms such as pain, heaviness, or fatigue.
- Duplex ultrasound confirming venous reflux.
- Evidence of valve dysfunction in veins.
- Failure of conservative treatments (e.g., compression stockings).
5 Major Insurance Providers in the USA for Vein Treatment Coverage!
Choosing the right insurance provider plays an important role in determining whether your vein treatment will be covered. In the United States, most major health insurance companies provide coverage for varicose vein procedures only when they are classified as medically necessary. This typically requires documented symptoms, diagnostic ultrasound results, and proof that conservative treatments have not worked.
Below are five of the most common insurance providers that often include coverage for vein treatments such as EVLT, RFA, and other medically approved procedures.
1. UnitedHealthcare (UHC)
UnitedHealthcare
One of the largest insurers in the U.S. often covers vein treatments when chronic venous insufficiency is documented.
Coverage strengths:
- Strong vascular procedure network.
- EVLT and RFA are commonly approved with pre-authorization.
- Requires ultrasound confirmation and symptom history.
2. Blue Cross Blue Shield (BCBS)
Blue Cross Blue Shield is a nationwide federation of independent insurers with varying state-level policies.
Coverage strengths:
- Wide coverage for medically necessary vein procedures.
- EVLT, RFA, and sclerotherapy are often included.
- Strict medical necessity requirements.
3. Aetna
Aetna generally follows clear clinical guidelines for vein treatment approval.
Coverage strengths:
- Covers venous ablation procedures when criteria are met.
- Requires failed conservative therapy first.
- Strong documentation and pre-authorization process.
4. Cigna
Cigna is well known for structured clinical policies and consistent approval rules.
Coverage strengths:
- Covers EVLT and RFA for symptomatic varicose veins.
- Requires duplex ultrasound evidence.
- Emphasis on medical necessity documentation.
5. Humana
Humana is popular for Medicare Advantage plans and vascular care coverage.
Coverage strengths:
- Frequently covers vein ablation for seniors.
- Strong emphasis on symptom-based eligibility.
- Requires prior authorization.
Does Insurance Cover VenaSeal for Varicose Veins?
Does insurance coverage include VenaSeal Varicose Veins treatment? Yes, insurance can cover VenaSeal for varicose veins, but only when it is considered medically necessary rather than a cosmetic procedure.
VenaSeal is a minimally invasive treatment used to close damaged veins caused by chronic venous insufficiency (CVI). Most insurance providers in the USA treat it similarly to other vein procedures like EVLT or radiofrequency ablation, meaning approval depends on medical evidence.
Insurance usually covers VenaSeal when:
- You have symptoms such as pain, swelling, or heaviness in the legs.
- Ultrasound confirms venous reflux (faulty vein valves).
- Conservative treatments like compression stockings have failed.
- A doctor documents the condition as medically necessary.
Insurance may NOT cover VenaSeal when:
- It is performed for cosmetic reasons only.
- There are no significant symptoms.
- Ultrasound does not show vein reflux.
- Conservative treatment has not been tried.
Important note: Some insurance companies may still require pre-authorization and in certain cases, prefer traditional treatments like EVLT or RFA before approving VenaSeal.
Frequently Asked Questions (FAQs)
Does insurance cover all vein treatments?
No. Insurance only covers treatments that are medically necessary, not cosmetic procedures.
How do I know if my treatment is medically necessary?
A vein specialist evaluates symptoms and ultrasound results to determine the necessity.
Does insurance cover VenaSeal?
Some insurance providers cover VenaSeal, but approval depends on policy and medical necessity.
What happens if insurance denies coverage?
You can appeal with additional documentation or explore payment plans.
How much will I pay with insurance?
Costs vary, but typically include deductibles, copays, and coinsurance.
References
- Almeida, J. I., Javier, J. J., Mackay, E. G., Bautista, C., & Proebstle, T. M. (2017). Thirty-six-month follow-up of first-in-human use of cyanoacrylate adhesive for treatment of saphenous vein incompetence. Journal of Vascular Surgery: Venous and Lymphatic Disorders, 5(5), 658–666. https://doi.org/10.1016/j.jvsv.2017.03.010
- Gibson, K., & Ferris, B. (2017). Cyanoacrylate closure of incompetent saphenous veins without postprocedure compression. Journal of Vascular Surgery, 65(1), 2–9. https://doi.org/10.1016/j.jvs.2016.08.069
- Morrison, N., Gibson, K., McEnroe, S., Goldman, M., King, T., Weiss, R., & Jones, A. (2015). Randomized trial comparing cyanoacrylate embolization and radiofrequency ablation. Journal of Vascular Surgery, 61(4), 985–994. https://doi.org/10.1016/j.jvs.2014.11.071
- Centers for Medicare & Medicaid Services. (2023). Treatment of varicose veins of the lower extremities. https://www.cms.gov
- Medtronic. (2023). VenaSeal closure system. https://www.medtronic.com