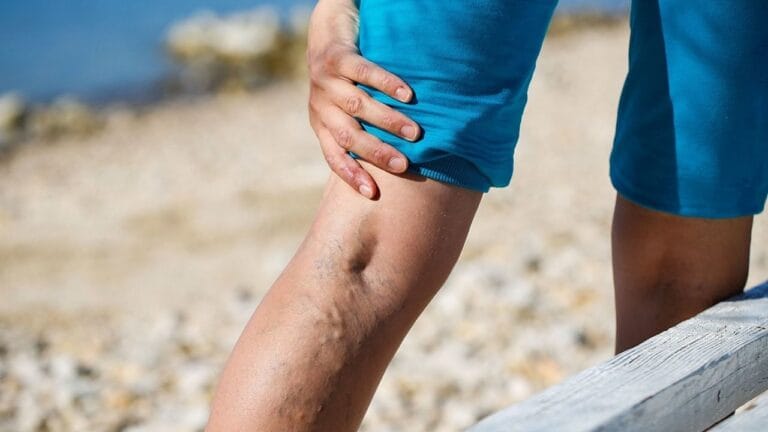
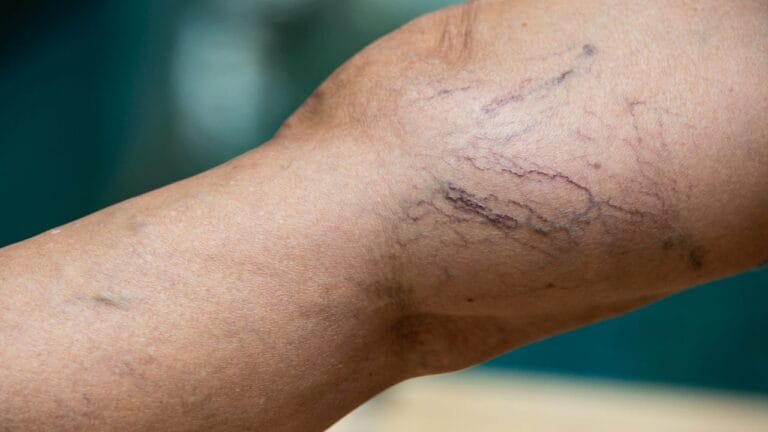
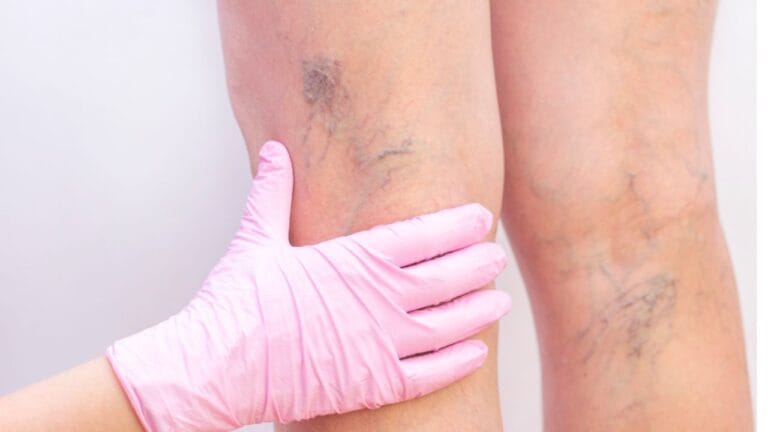
Varicose veins during pregnancy are a very common vascular condition affecting many expecting mothers worldwide. They occur when veins become enlarged, swollen, and twisted due to increased pressure in the circulatory system. Although usually not dangerous, they can significantly affect comfort, mobility, and quality of life during pregnancy.
This guide provides a deep, medically structured explanation of pregnancy-related varicose veins, including causes, symptoms, vulvar involvement, treatment options, postpartum recovery, and prevention strategies.
Let’s start-
Understanding Varicose Veins During Pregnancy
Well, let me clarify to you what varicose are veins at first. Varicose veins are dilated superficial veins that lose their normal ability to return blood efficiently to the heart. In pregnancy, the body undergoes major hormonal and circulatory changes that make vein walls more relaxed and valves less effective.

Normally, veins contain one-way valves that prevent backward blood flow. When these valves weaken, blood begins to pool in the lower limbs or pelvic area, leading to visible swelling and bulging.
During pregnancy, this condition most commonly affects: Legs (especially calves and thighs), Vulva (vulvar varicose veins) and Pelvic region. However, varicose veins during pregnancy happen because: Hormones relax vein walls, Blood volume increases, Growing uterus puts pressure on the veins. These changes slow down blood flow, causing blood to collect in veins and making them swell.
- Usually not dangerous
- Very common in pregnancy
- Often improves after delivery
- Can be managed with lifestyle changes and care
How Veins Normally Work
In a healthy body:
- Veins carry blood back to the heart.
- Small valves inside veins stop blood from flowing backward.
- Leg muscles help push blood upward against gravity.
This system keeps blood moving smoothly.
What Changes During Pregnancy
During pregnancy, the body goes through natural changes that affect blood circulation:
1. Hormonal Changes
- A hormone called progesterone increases.
- It relaxes the walls of blood vessels.
- Veins become softer and stretch more easily.
- Valves become weaker than normal.
2. Increased Blood Volume
- The body produces more blood to support the baby.
- Extra blood increases pressure inside the veins.
- Veins struggle to push blood back to the heart.
3. Pressure from the Growing Uterus
- The uterus becomes larger as the baby grows.
- It presses on the veins in the abdomen and pelvis.
- Blood flow from the legs slows down.
What Happens Because of These Changes?
When blood does not flow properly:
- Blood starts to pool in the veins.
- Veins become enlarged and visible.
- Pressure inside the veins increases.
- Swelling and discomfort may occur.
This condition is called varicose veins.
Common Areas Affected
Legs
- Most common area.
- Veins appear on calves and thighs.
- May cause heaviness, pain, or swelling.
Vulva (Genital Area)
- Can cause swelling or discomfort.
- Veins may be visible or tender.
- Often occurs in later pregnancy.
Pelvic Region
- Internal pressure or heaviness.
- Not always visible from the outside.
- Can cause discomfort while standing or walking.
These changes slow down blood flow, causing blood to collect in veins and making them swell.
Why Varicose Veins Develop During Pregnancy (Detailed Causes)?
What Causes Varicose Veins? Well, Varicose veins during pregnancy do not occur from a single cause. Instead, they result from a combination of hormonal, mechanical, genetic, and lifestyle factors.
- Hormonal changes (progesterone relaxes the vein walls).
- Increased blood volume (30-50% more blood in pregnancy).
- Uterine pressure on pelvic veins.
- Genetic predisposition.
- Lifestyle factors (standing, sitting long hours, and weight gain).
These factors slow blood flow and cause blood to pool in veins.
1. Hormonal Influence (Progesterone Effect)
One of the most important factors is increased progesterone levels during pregnancy. Progesterone relaxes smooth muscle tissue in blood vessel walls, making veins softer and more expandable. While this helps support pregnancy, it also weakens vein structure and valve function.
2. Increased Blood Volume (Physiological Adaptation)
During pregnancy, blood volume increases by almost 30-50% to support the developing fetus. This extra volume places additional stress on veins, especially in the lower body, where blood must work against gravity to return to the heart.
3. Uterine Pressure on Major Veins!
As the fetus grows, the uterus expands and compresses major pelvic veins, particularly the inferior vena cava. This compression slows down blood flow from the legs and pelvis, causing blood pooling and vein enlargement.
4. Genetic Predisposition:
Family history plays a strong role. If close relatives had varicose veins, weak vein walls may be genetically inherited, increasing risk during pregnancy.
5. Lifestyle and Physical Factors:
Certain daily habits can worsen the condition:
- Long hours of standing.
- Prolonged sitting without movement.
- Lack of physical activity.
- Excessive weight gain during pregnancy.
Symptoms of Varicose Veins in Pregnancy (Detailed Clinical Picture)
Symptoms vary in intensity depending on severity and stage of pregnancy.
Early Symptoms:
- Feeling of heaviness in legs.
- Mild discomfort after standing.
- Visible small vein patterns (spider veins).
Moderate Symptoms:
- Enlarged, twisted veins are visible under the skin.
- Swelling in feet and ankles.
- Aching pain, especially in the evenings.
- Burning or throbbing sensation.
Severe Symptoms:
- Constant leg discomfort.
- Skin discoloration around veins.
- Increased swelling during late pregnancy.
- Visible vein bulging even at rest.
These symptoms typically worsen in the third trimester when uterine pressure is highest.
Vulvar Varicose Veins During Pregnancy (Important Condition)!
Vulvar varicose veins occur when veins in the external genital area become enlarged due to pelvic pressure.
Causes:
- Increased pelvic blood flow.
- Compression of pelvic veins by the uterus.
- Weak venous valves in pelvic circulation.
Symptoms:
- Swelling in the vulva or labial area.
- Visible bluish or purplish veins.
- Pressure or fullness sensation.
- Discomfort while walking or standing for long periods.
- Pain during prolonged activity.
Clinical Note:
This condition is often underreported but is relatively common in the second and third trimesters. It usually resolves after childbirth.
Varicose Veins Pregnancy Treatment (Safe & Medical Options)
Varicose veins during pregnancy usually focus on symptom control rather than permanent removal, because most medical procedures are avoided during pregnancy for safety reasons.
Treatment aims to improve blood circulation, reduce swelling, and relieve discomfort. In cases where symptoms become severe or require expert evaluation, consultation with a vascular specialist is recommended.
For professional varicose vein treatment, I mean for assessment and advanced care, patients can consult a specialist for personalized varicose vein management and pregnancy-safe treatment guidance.
However, Treatment during pregnancy focuses on symptom management and improving circulation, not surgical correction.
1. Compression Therapy (Most Effective First-Line Treatment)
Medical-grade compression stockings improve venous return by applying graduated pressure to the legs. This reduces swelling, prevents blood pooling, and relieves pain.
2. Physical Activity and Circulation Improvement
Regular movement is essential:
- Walking improves calf muscle pump function
- Prenatal yoga enhances circulation
- Gentle stretching reduces venous pressure
3. Leg Elevation Technique
Elevating legs above heart level for 15–20 minutes several times a day helps reduce venous pressure and swelling.
4. Position Management
- Avoid standing for long periods
- Avoid sitting with crossed legs
- Sleep on the left side to reduce pressure on the inferior vena cava
5. Cold Therapy
Applying cold compresses can temporarily reduce swelling and discomfort.
Important Medical Note:
Invasive treatments like laser therapy, vein stripping, or sclerotherapy are generally avoided during pregnancy unless medically necessary.
Varicose Veins After Pregnancy (Recovery Phase)
After childbirth, many hormonal and mechanical pressures resolve naturally.
Natural Recovery Process:
- Blood volume gradually returns to normal.
- Uterine pressure disappears.
- Hormone levels stabilize.
As a result, many women experience:
- Significant reduction in vein size.
- Decrease in pain and heaviness.
- Partial or complete disappearance of symptoms.
When Symptoms Persist:
If varicose veins remain 3-6 months postpartum, medical treatment may be required:
- Sclerotherapy (injection treatment).
- Laser vein therapy.
- Minimally invasive procedures.
When to Take Specialist Consultation?
Although pregnancy varicose veins are often harmless, medical consultation is important in certain situations to ensure maternal safety and prevent complications.
You should consult a specialist if:
- Pain becomes persistent or severe.
- One leg shows sudden or significant swelling.
- Veins become hard, red, or warm to the touch.
- Skin discoloration or ulcers develop near affected veins.
- Symptoms interfere with daily activities or sleep.
- Vulvar varicose veins cause significant discomfort or pressure.
- No improvement is seen after delivery (postpartum period).
For expert evaluation and advanced vascular care, consultation with Dr. Rema Malik is recommended. A specialist assessment can help determine severity, rule out complications like deep vein thrombosis, and provide personalized treatment planning for safe pregnancy and postpartum recovery.
Prevention Strategies (Highly Important for At-Risk Mothers)
Prevention is especially effective when started early in pregnancy.
Lifestyle Prevention:
- Regular walking (20-30 minutes daily).
- Avoid prolonged immobility.
- Maintain a healthy pregnancy weight gain.
- Avoid tight clothing around the waist and thighs.
Circulatory Support:
- Use compression stockings from early pregnancy.
- Stay hydrated to improve blood flow.
- Elevate legs frequently.
Posture Awareness:
- Avoid standing in one position too long.
- Change posture every 30-40 minutes.
- Sleep on the left side for better venous return.
Conclusion
Varicose veins during pregnancy are a natural result of hormonal and physical changes in the body. While they can be uncomfortable, they are generally manageable and often temporary.
With proper care, such as compression therapy, exercise, posture control, and lifestyle adjustments, most women experience significant relief during pregnancy and full recovery after childbirth.
So, understanding conditions like pregnancy, varicose veins, vulvar varicose veins, and varicose veins after pregnancy helps ensure better awareness, early management, and improved maternal comfort.
References
- American College of Obstetricians and Gynecologists. (2021). Pregnancy and varicose veins. ACOG Patient Education. https://www.acog.org
- Bergan, J. J., Schmid-Schönbein, G. W., Smith, P. D., Nicolaides, A. N., Boisseau, M. R., & Eklof, B. (2006). Chronic venous disease. New England Journal of Medicine, 355(5), 488–498. https://doi.org/10.1056/NEJMra055289
- Gillet, J. L., Perrin, M., & Allaert, F. A. (2007). Short- and long-term outcomes of pregnancy-related varicose veins. Journal of Vascular Surgery, 46(3), 474–480. https://doi.org/10.1016/j.jvs.2007.04.036
- Katz, V. L. (2012). Comprehensive gynecology (6th ed.). Elsevier.
- Kisner, C., & Colby, L. A. (2017). Therapeutic exercise: Foundations and techniques (7th ed.). F.A. Davis Company.
- National Health Service (NHS). (2023). Varicose veins in pregnancy. https://www.nhs.uk
- Society for Vascular Surgery. (2022). Varicose veins and chronic venous disease. https://vascular.org
- UpToDate. (2024). Varicose veins of the lower extremities in pregnancy. Wolters Kluwer. https://www.uptodate.com