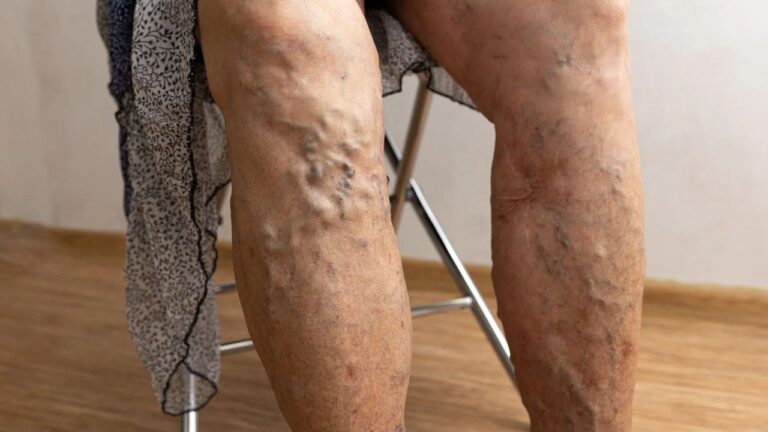
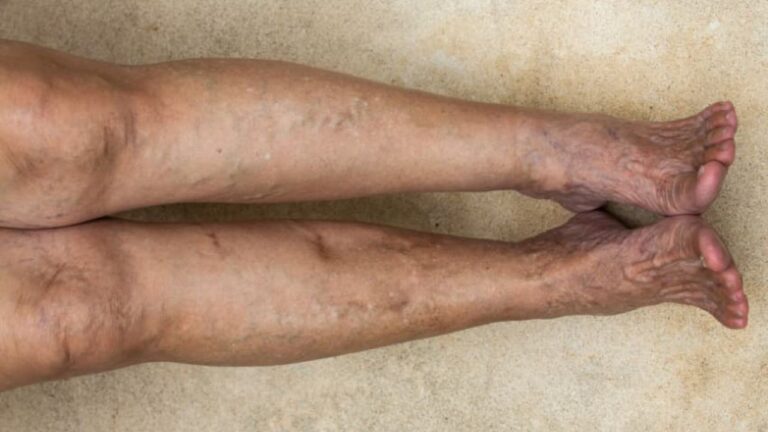
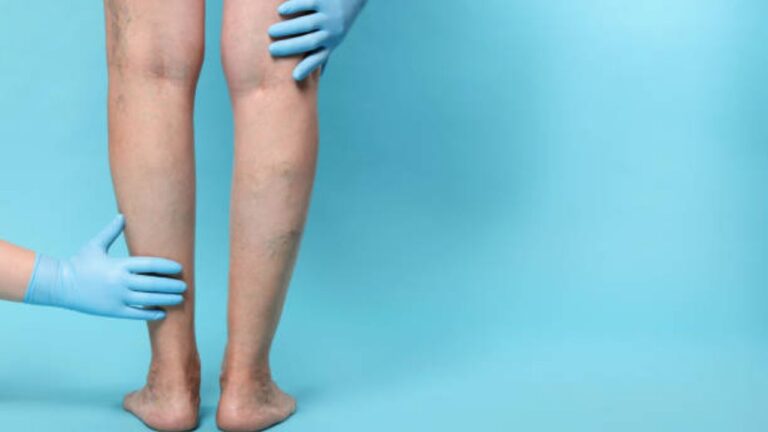
Sarah, a 55-year-old teacher from Ohio, had always been active. She loved walking her dog every morning and standing at her classroom for hours, helping students. But over the years, she noticed her legs feeling heavier and more swollen by the end of the day. Tiny veins started twisting around her calves, and dark patches appeared near her ankles. At first, she ignored it, thinking it was just part of getting older.
Years later, after visiting a vein specialist, Sarah learned she had chronic venous insufficiency (CVI) a condition where the veins in the legs cannot efficiently send blood back to the heart. While CVI itself is rarely life-threatening, untreated cases can lead to discomfort, ulcers, and other complications. The good news is that with early awareness, simple lifestyle changes, and expert guidance, people like Sarah can manage their symptoms and protect their leg health for life.
This story reminds us that venous health is something to care for every day, not just when pain or swelling appears. Understanding CVI, its risks, and ways to prevent complications is the first step toward healthier legs and a better quality of life.
Look below to get the in-depth discussion of today’s session-
How does CVI develop?
Vein valves act as one-way gates that push blood back toward the heart. These valves ensure blood flows upward and prevent it from pooling in the legs. When the valves weaken or fail, blood can start to flow backward, a process called venous reflux. This increases pressure inside the veins, stretching the vein walls and causing damage over time.
CVI develops gradually through several stages:
Step 1: Valve weakening
Vein valves lose strength due to aging, genetics, or prolonged pressure from standing or sitting.
Step 2: Backward blood flow
Failed valves allow blood to flow backward and pool in the lower legs.
Step 3: Increased venous pressure
Blood pooling increases pressure in the veins, stretching them further and worsening valve damage.
Step 4: Vein enlargement and varicose veins
High pressure causes veins to bulge or twist, forming varicose veins.
Step 5: Swelling and fluid buildup
Excess pressure forces fluid into surrounding tissues, causing leg swelling (edema).
Step 6: Skin changes and ulcers
Over time, pressure and poor blood flow can lead to skin discoloration, thickening, or painful venous ulcers, especially near the ankles.
CVI is very common in adults. Studies show that up to 40% of U.S. adults have some form of chronic venous disease, and about 6-7% experience more severe symptoms like leg ulcers. Risk factors include age, obesity, pregnancy, prolonged sitting or standing, and family history.
Early detection is key. Identifying CVI in its initial stages can reduce discomfort, prevent swelling, and lower the risk of complications. Addressing problems early gives the best chance for healthy, comfortable legs over time.
What Can Chronic Venous Insufficiency Lead To?
Chronic venous insufficiency (CVI) can begin with very mild, almost unnoticeable symptoms, such as slight leg swelling, heaviness, or occasional fatigue after long periods of standing. At first, these changes may seem minor and easy to ignore. However, if CVI is left untreated, the condition can gradually progress, and the pooling of blood in the lower legs increases venous pressure, leading to more noticeable and sometimes serious complications.
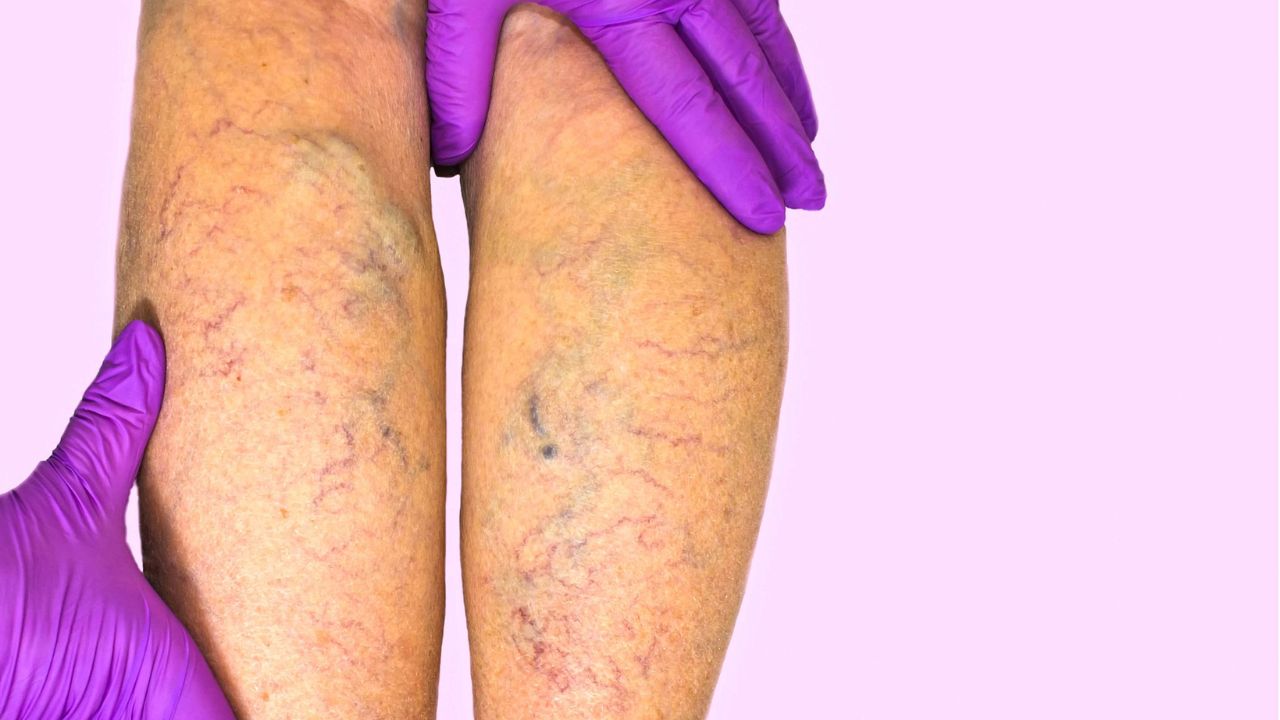
Some of the most common consequences of untreated CVI include:
- Swelling (edema): Fluid often accumulates in the lower legs, particularly around the ankles. Swelling usually worsens by the end of the day or after prolonged standing, causing discomfort and a feeling of heaviness.
- Varicose veins: The increased venous pressure stretches veins, causing them to bulge, twist, and become visibly enlarged. These veins may appear blue or dark purple and can lead to aching or throbbing sensations.
- Skin changes: Over time, chronic pressure and poor blood flow can damage the skin. This may appear as brown discoloration, dryness, or thickening, most often around the ankles, and can sometimes develop into eczema or inflammation.
- Venous ulcers: In 1-5% of severe CVI cases, open sores called venous ulcers may develop. These sores are slow to heal, often painful, and can become infected if left untreated.
- Pain, heaviness, and fatigue: Affected legs may feel tired, heavy, or achy, particularly after walking, standing, or at the end of the day.
- Infection risk: Open ulcers or damaged skin increase the risk of infections. Prompt care is essential to prevent further complications.
- Rare but serious risks: In some cases, CVI can be associated with deep vein thrombosis (DVT), where a blood clot forms in a deep vein. DVT can be life-threatening if a clot breaks loose and travels to the lungs.
Managing CVI early is key to preventing these complications. Compression therapy, regular exercise, leg elevation, and professional care can slow the progression of the disease, reduce swelling, improve circulation, and improve overall quality of life.
Key Points to Remember:
- Swelling and varicose veins are common early signs of CVI.
- Severe CVI can cause skin changes and painful venous ulcers.
- Early treatment reduces the risk of infection and DVT.
- Lifestyle adjustments and compression therapy are essential for preventing complications.
By recognizing these signs and taking action early, patients can maintain healthier legs, reduce discomfort, and prevent serious complications, keeping mobility and daily life as normal as possible.
Treatment and Preventive Care
Lifestyle measures play a major role in controlling CVI. Walking regularly activates the calf muscles, which pump blood upward. Elevating legs after long periods of sitting or standing reduces swelling. Maintaining a healthy weight lowers pressure on the veins.
Compression stockings support circulation and prevent blood from pooling in the lower legs. They are especially useful for people at higher risk, including pregnant women, people with physically demanding jobs, or those with varicose veins.
For patients with persistent symptoms or advanced CVI, minimally invasive procedures are highly effective. Endovenous laser therapy (EVLT) and sclerotherapy can close faulty veins. Laser therapy forces blood to reroute through healthier veins, relieving symptoms and reducing long-term complications. Recovery is usually quick, and most patients feel relief soon after the procedure.
If you are unsure where to start, it’s important to know who treats venous insufficiency. Vascular specialists, interventional radiologists, and vein experts can evaluate your veins, recommend appropriate treatments, and guide you on preventive measures to avoid progression. Early consultation ensures better outcomes and lasting relief.
Professional Guidance and Expert Care
Knowing the right specialists is crucial for proper management of venous insufficiency. Vascular surgeons, interventional radiologists, and vein experts can check how well your veins are working. They can detect problems early, explain treatment options, and create a plan tailored just for you.
Early professional guidance helps prevent complications, control swelling, and improve mobility. Specialists can also advise on preventive strategies, the correct compression levels, and follow-up care to keep your veins healthy over time.
For trusted, patient-centered care, Dr. Rema Malik is recognized for her expertise in vascular and vein health. She emphasizes early detection, combines lifestyle guidance with medical interventions, and ensures patients receive long-term support for optimal vein health.
Conclusion: Protecting Your Veins for the Long Term
Chronic venous insufficiency may start with mild swelling or discomfort, but it can get worse if ignored. With simple lifestyle changes, compression therapy, expert guidance, and minimally invasive treatments, most people can manage symptoms effectively.
However, the key is early awareness. Taking care of your veins today helps prevent complications, keeps your legs comfortable, and supports mobility. Healthy veins mean stronger, more active legs for years to come.
So that’s all on what chronic venous insufficiency can lead to
Frequently Asked Questions (FAQ)
Can CVI be fatal?
CVI itself is rarely fatal. Complications like ulcers or DVT are more serious but can be prevented with early care.
What are the first signs of CVI?
Swelling, heaviness, varicose veins, and skin changes around the ankles are early indicators.
Does laser therapy work for varicose veins?
Yes. Laser therapy closes diseased veins and redirects blood through healthier veins. Recovery is fast, and symptoms improve quickly.
Who should I see for venous insufficiency?
Vascular specialists, interventional radiologists, or vein experts can evaluate and treat CVI. Early consultation improves outcomes.
References
- Society for Vascular Surgery Chronic Venous Disease Guidelines
- American Venous Forum – Vein Health and Treatment Recommendations
- National Institutes of Health (NIH) – Chronic Venous Insufficiency Overview
- Cleveland Clinic – Varicose Veins and Venous Disorders
- Mayo Clinic – Chronic Venous Insufficiency: Causes, Symptoms, and Treatment