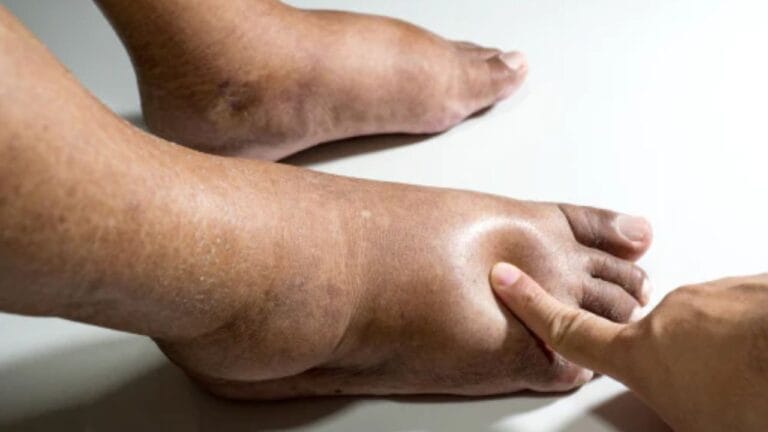
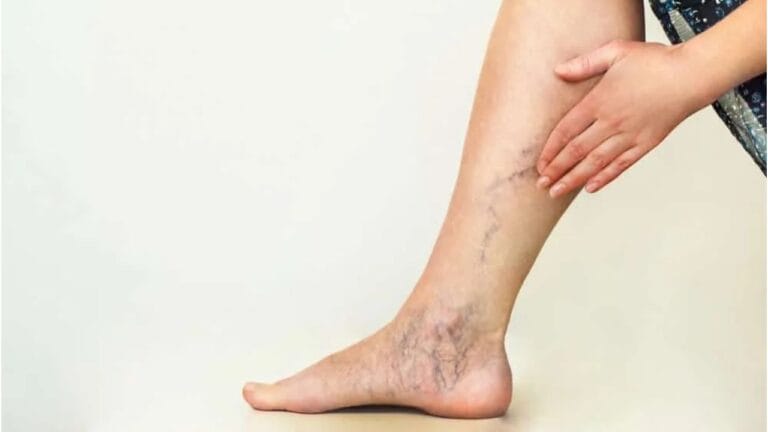
Venous insufficiency isn’t just about veins that look twisted or bulging—it’s a real condition that can affect how well blood flows through your legs, impact your skin, and even make moving around uncomfortable. The tricky part is that it usually develops slowly, so many people don’t realize they need medical help—or aren’t sure who to see.
Getting the right care early is key. The right specialist can help manage symptoms, prevent skin problems, painful sores, infections, and keep your legs feeling healthy and mobile. Knowing who treats venous insufficiency and what they do makes it easier to get the right help before small issues turn into bigger problems.
Let’s see the brief discussion of this topic-
Medical Specialists Who Treat Venous Insufficiency
Venous insufficiency is primarily treated by physicians who specialize in vascular and venous disorders. These specialists have advanced training in diagnosing blood flow problems and managing both early and advanced disease.
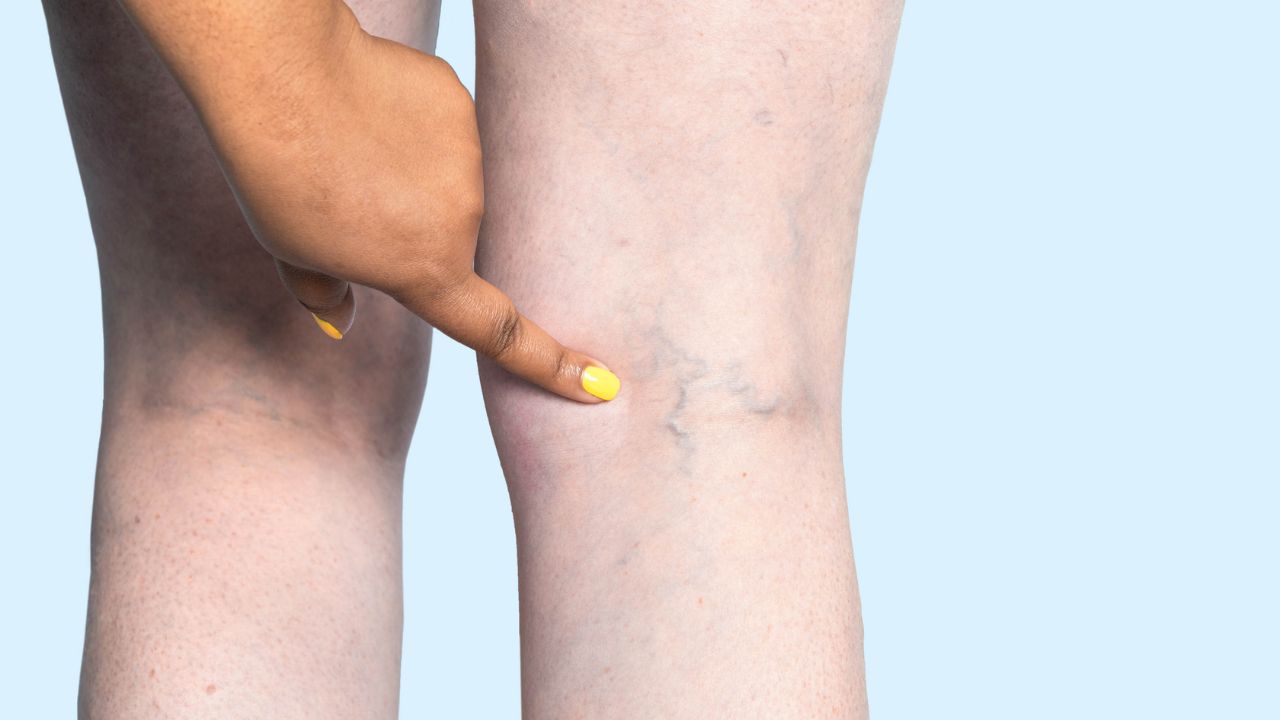
Vascular Surgeons
Vascular surgeons are the most comprehensive specialists for venous insufficiency. Despite their title, they treat a wide range of vein conditions using both non-surgical and minimally invasive techniques.
They are uniquely qualified to:
- Perform detailed vascular evaluations.
- Interpret duplex ultrasound imaging.
- Diagnose valve dysfunction and venous reflux.
- Manage advanced cases with skin changes or ulcers.
- Offer procedural and long-term treatment plans.
Patients with chronic swelling, skin discoloration, or non-healing leg wounds often benefit most from evaluation by a vascular surgeon, as these symptoms indicate more advanced disease.
Interventional Radiologists
Interventional radiologists specialize in image-guided treatments for vascular conditions. They use advanced imaging technology to identify abnormal blood flow patterns and treat affected veins through small, minimally invasive approaches.
Their expertise is particularly valuable for:
- Complex venous anatomy
- Patients who are not surgical candidates
- Advanced venous reflux requiring catheter-based treatment
- Recurrent venous disease after prior procedures
Interventional radiologists often work alongside vascular surgeons to ensure precise diagnosis and targeted treatment.
Phlebologists (Vein Specialists)
Phlebologists focus exclusively on vein disorders, including venous insufficiency and varicose veins. They commonly treat patients in earlier stages of disease or those with moderate symptoms.
Their care typically includes:
- Clinical evaluation of leg symptoms.
- Compression therapy guidance.
- Lifestyle and activity counseling.
- Office-based vein treatments.
- Ongoing symptom monitoring.
Phlebologists play an important role in early intervention, helping slow disease progression before complications develop.
Primary Care Providers (First Point of Contact)
Primary care physicians are often the first doctors patients consult when leg swelling or discomfort appears. While they do not manage venous insufficiency long-term, they are essential for early recognition.
They help by:
- Evaluating leg swelling and ruling out other causes.
- Identifying risk factors such as obesity or prior blood clots.
- Initiating referrals to vein specialists.
- Coordinating overall patient care.
Persistent or worsening symptoms should always prompt referral to a vascular or vein specialist.
Does Venous Insufficiency Cause Edema?
Does venous insufficiency cause edema? Yes, venous insufficiency is a leading cause of chronic leg edema. When vein valves fail, blood pools in the lower extremities instead of flowing efficiently back to the heart. This pooling increases pressure inside the veins, forcing fluid out of blood vessels and into surrounding tissues.
Specialists focus on edema because:
- It reflects worsening venous pressure.
- It accelerates skin and tissue damage.
- It increases the risk of ulcers and infection.
- It directly affects comfort and mobility.
Controlling edema is often the primary goal of venous treatment, and improvement in swelling is a key indicator of treatment success.
When Venous Insufficiency Becomes a Serious Condition
Venous insufficiency is often underestimated because it progresses slowly and may initially seem harmless. However, untreated disease causes chronic inflammation and tissue injury, leading to significant complications over time.
Advanced disease may result in:
- Thickened, hardened skin.
- Dark discoloration around the ankles.
- Open venous ulcers.
- Recurrent skin infections.
- Reduced walking tolerance and independence.
This progression underscores why venous insufficiency should be treated as a medical condition, not merely a cosmetic concern.
How Specialists Determine the Right Treatment Plan
Venous specialists take a comprehensive, individualized approach when treating venous insufficiency. They assess not just visible veins, but the entire venous system and patient lifestyle.
Key evaluation factors include:
- Degree of valve dysfunction.
- Presence and severity of edema.
- Skin integrity and ulcer risk.
- History of blood clots.
- Occupational and mobility demands.
Treatment plans are designed to control symptoms, reduce pressure, and prevent progression, rather than simply treating visible veins.
Expert Clinical Perspective
According to Dr. Rema Malik, venous insufficiency isn’t just a minor vein problem-it should always be treated as a progressive vascular disease. Many patients don’t realize how serious it can become and often wait until swelling, pain, or skin changes are already noticeable before seeking medical help. By the time they see a specialist, some of the simpler, more effective treatment options may no longer be as helpful.
Dr. Malik emphasizes that early intervention makes a huge difference in outcomes. Seeing a vascular or vein specialist at the first signs of discomfort or visible vein changes can help manage symptoms effectively and prevent the condition from worsening. Early treatment focuses on controlling edema, reducing the risk of venous ulcers, preserving skin and nerve health, and maintaining long-term mobility.
In her experience, patients who act early and follow a personalized treatment plan experience less pain, better leg function, and a significantly lower chance of serious complications. She stresses that venous insufficiency is not something to ignore, even if symptoms seem minor at first. Proper specialist care gives patients the best chance to keep their legs healthy, active, and comfortable for years to come.
Dr. Malik’s perspective clearly shows that timely and specialized care is the cornerstone of successful CVI management and that understanding the disease early can prevent unnecessary suffering and long-term complications.
When to Seek a Venous Specialist
Patients should seek specialist evaluation if they notice:
- Persistent leg or ankle swelling
- Heaviness or aching after standing
- Skin color changes or thickening
- Visible veins with symptoms
- Slow-healing wounds near the ankles
Early treatment reduces the need for complex interventions later.
Can Chronic Venous Insufficiency Be Fatal?
Can chronic venous insufficiency be fatal? Chronic venous insufficiency itself is rarely directly fatal, but its complications can pose serious health risks if ignored.
Potential dangers include:
- Severe infections from open ulcers.
- Blood clot formation due to impaired circulation.
- Reduced mobility leading to cardiovascular decline.
- Systemic illness from chronic wounds.
Specialist care focuses on preventing these complications long before they become life-threatening.
Final Takeaway
Venous insufficiency is best treated by vascular surgeons, interventional radiologists, and dedicated vein specialists, often working together. While primary care providers play a vital role in early detection, definitive diagnosis and management require specialized vascular expertise.
Because venous insufficiency commonly causes chronic edema and can lead to serious complications if untreated, early specialist care is essential for protecting leg health, mobility, and overall quality of life. So don’t worry, just try to consult with an expert when you see the symptoms of venous insufficiency!
Frequently Asked Questions (FAQ)
Which doctor should I see first for venous insufficiency?
A vascular surgeon or vein specialist is the best choice, especially if swelling, skin changes, or pain are present. Early consultation helps prevent complications and ensures treatment starts before symptoms worsen.
Can venous insufficiency be treated without surgery?
Yes. Many patients are managed with compression therapy, lifestyle changes, and minimally invasive procedures. These approaches often provide significant relief and slow disease progression without the need for major surgery.
How is venous insufficiency diagnosed?
Diagnosis typically involves a physical exam and duplex ultrasound to assess blood flow and valve function. Accurate diagnosis is important to guide the most effective treatment plan for each patient.
Is leg swelling always caused by venous insufficiency?
No. Swelling can also be caused by heart, kidney, or lymphatic conditions, which is why medical evaluation is important. Proper assessment ensures the right underlying cause is identified and treated promptly.
When is venous insufficiency considered advanced?
Advanced disease includes persistent edema, skin discoloration, thickening, or open venous ulcers. At this stage, more intensive management is usually needed to prevent serious complications and maintain mobility.
References
- Eberhardt RT, Raffetto JD. Chronic Venous Insufficiency. Circulation.
- Society for Vascular Surgery. Clinical Practice Guidelines for Chronic Venous Disease.
- American Venous Forum. Venous Insufficiency Treatment Standards.
- Cleveland Clinic. Venous Insufficiency: Causes, Symptoms, and Treatment.
- National Heart, Lung, and Blood Institute (NHLBI). Venous Disorders Overview.