During surgery, dried blood on the skin surface is very common. After surgery, the skin becomes more sensitive than usual. Post-surgical skin is very fragile, and rubbing the skin or using harsh products after surgery can irritate the skin, slow recovery, increase discomfort, damage new tissue, and increase the risk of infection.
That’s why skin should not be pulled immediately after surgery. Moreover, the skin surface should be cleaned with caution and care, followed by continuous observation to confirm the presence of any infection. Proper blood removal from the skin is a stepwise approach that needs to be done one step after another.
Let’s move on to the article to get the procedure of blood removal in the best scientific way.
What Causes Dried Blood on the Skin?
During surgery, small blood vessels known as capillaries are cut, which leads to bleeding around the incision site. As the blood is exposed to air, it undergoes coagulation—a natural biological process where fibrin proteins form a mesh that traps blood cells. This creates a clot that gradually hardens and dries on the skin’s surface.
According to the National Institutes of Health (NIH), coagulation is a vital protective mechanism. It helps stop excessive bleeding, forms a temporary barrier against bacteria, and supports the body’s natural wound-healing process. Dried blood on the skin after surgery is, therefore, a normal part of recovery.
Why Gentle Care Matters?
Healing skin is extremely delicate, especially in the days following surgery. Removing dried blood aggressively can irritate the skin, reopen healing tissue, delay recovery, or increase the risk of infection. Surgical aftercare references, including the Sabiston Textbook of Surgery, emphasize minimizing trauma to both the wound edges and the surrounding skin to support optimal healing.
What Science Says?
- Warm, gentle cleansing helps maintain wound hygiene without disrupting newly forming tissue.
- Harsh scrubbing, alcohol, or strong antiseptics can damage healing cells and increase scarring.
- Mild solutions and clean techniques are preferred over aggressive products in most postoperative care.
What You Should Know Before Cleaning
Your incision site is not the same as regular skin and should never be treated like a normal skincare routine. Clinical wound-care guidelines stress that improper cleaning can do more harm than good.
Principles of Safe Cleaning
- Use mild solutions: Normal saline or mild soap with water; avoid alcohol or hydrogen peroxide on open wounds unless advised by your clinician.
- Use soft materials only: Sterile gauze or a soft, clean cloth to prevent skin trauma.
- Avoid scrubbing: Scrubbing can damage delicate tissue, delay healing, and increase infection risk (as noted in clinical reviews on PMC).
Clinical wound-care studies also note that while practices may vary among healthcare professionals, gentle cleansing to remove crusting and dried blood is a widely accepted, evidence-based approach to postoperative care.
Step-by-Step: Removing Dried Blood Safely
After surgery, dried blood can cling firmly to the skin around the incision, making removal feel uncomfortable or even risky. The most important rule is never to rush or scrub. Surgical skin is fragile, and improper cleaning can disrupt healing tissue, reopen the wound, or introduce infection.
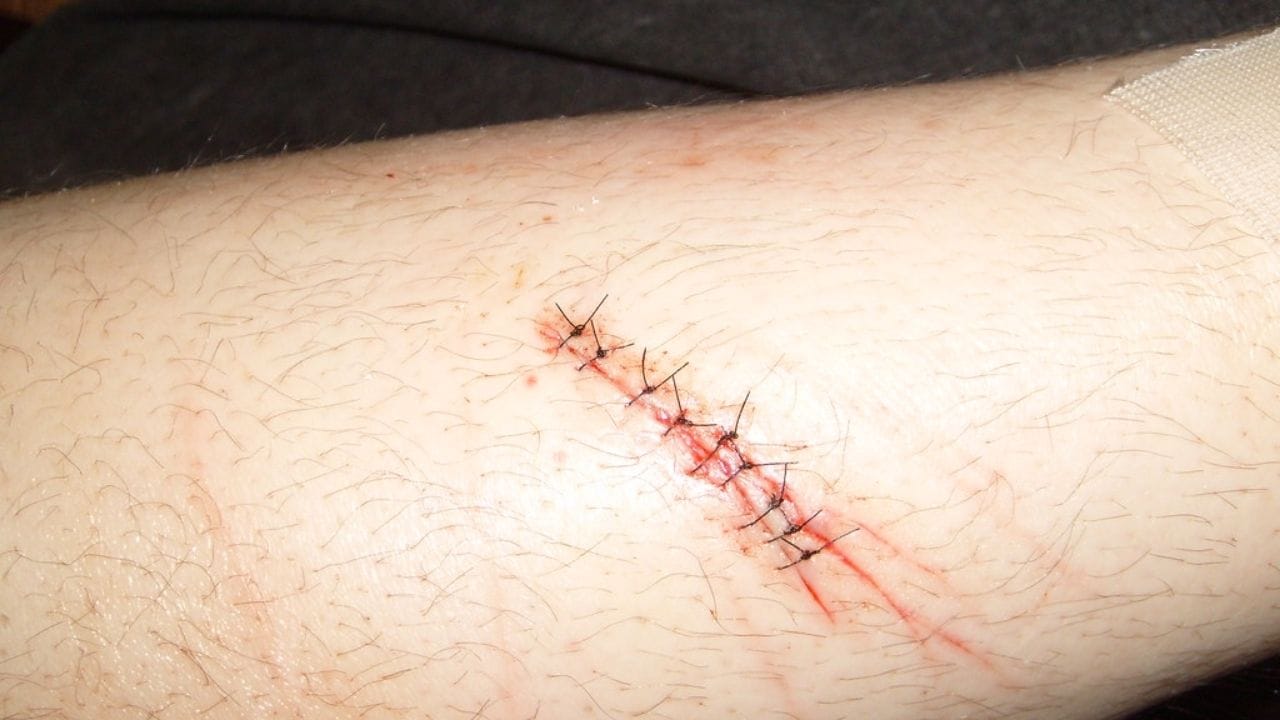
The steps below follow evidence-based wound-care principles used in clinical settings and are designed to remove dried blood gently, safely, and without harming newly healing skin. Each step focuses on softening first, minimizing friction, and protecting the incision area throughout the process.
Step 1: Soften the Crust First
Before removal, soften the dried blood. Soak a cloth in lukewarm saline or warm water. Warm water increases moisture, helps loosen dried blood by softening the fibrin structure holding it to the skin. Hold it in the area for 5–10 minutes. It makes crusts easier to remove without force. Heat increases molecular movement and mildly softens protein bonds, reducing the need for mechanical force. As a result, soft crusts can be wiped away, not ripped off.
This approach aligns with principles from the American Association of Wound Care – Wound Cleansing.
Step 2: Use Mild, pH-Balanced Soap
A gentle cleanser helps remove organic residue without harming skin cells. Healthy skin has a slightly acidic pH (~5.5). Harsh soaps disrupt the skin barrier, increasing irritation and infection risk. The American Academy of Dermatology’s Proper Wound Cleaning recommends fragrance-free, non-irritating cleansers.
Step 3: Gently Remove with Fingertips
Apply mild soap to a soft, damp washcloth. Lightly massage the area using clean fingertips or a very soft cloth. Pat and dab gently move from the outer edges inward. Don’t scrub it can damage newly forming skin. Rinse with warm water. Excessive friction can damage migrating keratinocyte cells essential for wound closure (NIH). Avoid scrubbing tools, loofahs, or fingernails.
Step 4: Dry and Protect
Pat dry with a clean towel or sterile gauze. Patting removes moisture without disturbing healing tissue. Leftover soap residue can increase trans epidermal water loss (TEWL), which weakens the skin barrier. Apply a thin layer of petroleum jelly or prescribed ointment. Cover with a non-stick bandage if recommended by your clinician. This protects the area and supports moist wound healing, a cornerstone of modern wound care.
Step 5: Optional protective layer (if allowed)
If your doctor approves, apply a thin layer of petroleum jelly or antibiotic ointment to keep skin moist. Cover with a fresh, sterile bandage if the wound is still exposed. Moisture prevents cracking, reduces itching, and protects the incision from friction or clothing.
For professional guidance on post-surgical wound care, consult DR. REMA MALIK. She provides personalized advice on wound management and ensures proper healing techniques are followed. Following expert guidance can help prevent complications, minimize scarring, and support faster recovery after surgery.
What Not to Do?
Just as important as knowing how to clean dried blood is understanding what should be avoided during postoperative care. Healing skin and incision sites are highly sensitive, and certain common habits or products can unintentionally delay healing, increase infection risk, or worsen scarring. The following precautions are based on modern wound-care principles that prioritize protecting fragile tissue and minimizing unnecessary trauma.
Avoid Harsh Substances
Products such as hydrogen peroxide, iodine, alcohol, and strong antiseptics may seem effective, but when misused, they can damage healthy skin cells and slow the healing process. These substances can be too harsh for healing tissue and are generally not recommended unless specifically directed by a healthcare provider.
Avoid Picking or Scraping
Forcefully picking at dried blood or scabs can interfere with natural healing and cause complications. This can:
- Reopen healing tissue
- Increase the risk of infection
- Lead to more noticeable scarring
If dried blood is present in hair near the incision, use a minimal amount of mild shampoo and rinse gently. Avoid direct rubbing or scrubbing over the incision area. Modern wound-care education strongly emphasizes avoiding mechanical trauma to wounds unless debridement is medically necessary and performed under professional supervision.
Specialized Treatments
Some patients with slow-healing wounds or underlying circulatory issues may benefit from specialized interventions. Varicose Vein Treatment provides advanced care for visible, painful veins that can impair healing and affect overall circulation.
Well, treatment options can include minimally invasive procedures such as endovenous laser therapy, radiofrequency ablation, or sclerotherapy to improve blood flow. Proper management of varicose veins reduces swelling, prevents complications, and supports faster recovery of post-surgical or chronic wounds. Lifestyle adjustments, compression therapy, and expert monitoring further enhance outcomes for patients with venous insufficiency.
Recognizing Trouble Signs
Even with proper care, it is important to stay alert for signs that something may be wrong. Contact your surgeon or healthcare provider promptly if you notice:
- New or persistent bleeding
- Increasing redness, warmth, or swelling
- Pus, unusual discharge, or foul odor
- Fever or chills
These symptoms may indicate infection or other postoperative complications and should be evaluated by a medical professional. For expert guidance, consult DR. REMA MALIK to ensure proper wound assessment and safe recovery.
Vein Health: Varicose Vein Care
If you have varicose veins, they may impact circulation and healing. Early management is key to avoiding complications after surgery. Learn more about Varicose Vein Treatment to improve vein health and support recovery.
Vein Health: Chronic Venous Insufficiency (CVI)
Chronic venous insufficiency can slow healing and increase swelling or discomfort around surgical sites. Professional care is recommended to maintain optimal circulation and reduce complications. Explore Chronic Venous Insufficiency (CVI) Treatment for tailored solutions.
Final Thoughts
After surgery, proper blood removal is the priority and must be done very cautiously. It will accelerate your body’s healing when you approach dried blood removal with care, patience, and respect for medical evidence, with the primary objective of cleanliness. Careful considerations must be made during cleaning by avoiding harsh antiseptics, aggressive scrubbing, or picking at scabs, as these can damage healthy tissue and increase the likelihood of infection and scarring. If you ever suspect the process, checking with your surgeon or wound care specialist is always the best step.
FAQ
How long does dried blood last after surgery?
Usually, a few days. As healing progresses and you clean gently, it should gradually disappear.
Can I shower after surgery?
Most people can shower within 24-48 hours, but always follow your surgeon’s instructions. Avoid soaking unless cleared.
What if the dried blood won’t come off?
Don’t force it. Keep softening it over multiple sessions. If it’s stuck or painful, leave it and ask your doctor.
Is dried blood a sign of infection?
No! Dried blood alone is normal. Infection signs include increasing redness, warmth, swelling, pus, or fever.
Can I use cotton pads or tissues?
Avoid anything that sheds fibers. Use soft cloths or sterile gauze only.
References:
- Smeltzer, S. C., Bare, B. G., Hinkle, J. L., & Cheever, K. H. (2020). Brunner & Suddarth’s textbook of medical-surgical nursing (14th ed.). Wolters Kluwer.
- World Health Organization (WHO). (2018). Global guidelines for the prevention of surgical site infection.
- MedlinePlus (U.S. National Library of Medicine). (2024). Surgical wound care.
- Ousey, K., & McIntosh, C. (2010). Topical antimicrobial agents for the treatment of chronic wounds. Journal of Wound Care, 19(8), 325–330.
- Doherty, G. M. (Ed.). (2021). Current diagnosis & treatment: Surgery (15th ed.). McGraw-Hill Education