Ever notice your legs feel heavier than usual after a day of work, or that veins seem to stand out more than before? Oh, it might feel like just getting older, right? But sometimes, your legs are trying to tell you something important. Chronic venous insufficiency (CVI) is a condition that develops slowly, often without pain at first, but if ignored, it can affect your mobility, comfort, and even lead to complications over time.
Many people brush off swelling, dark patches near the ankles, or varicose veins as “normal aging.” Aww, but recognizing the early signs can make all the difference. With the right care, CVI can be managed effectively, keeping your legs healthy and comfortable for years to come.
Lets see brief discussion about whether chronic venous insufficiency or not-
What Is Chronic Venous Insufficiency?
Chronic venous insufficiency, or CVI, happens when the tiny valves in your leg veins don’t work as they should. Normally, these valves act like one-way gates, pushing blood back up toward the heart. But when they weaken or fail, blood can flow backward and start pooling in the lower legs. Over time, this increases pressure inside your veins, stretching their walls and causing discomfort, swelling, and visible changes in your legs.
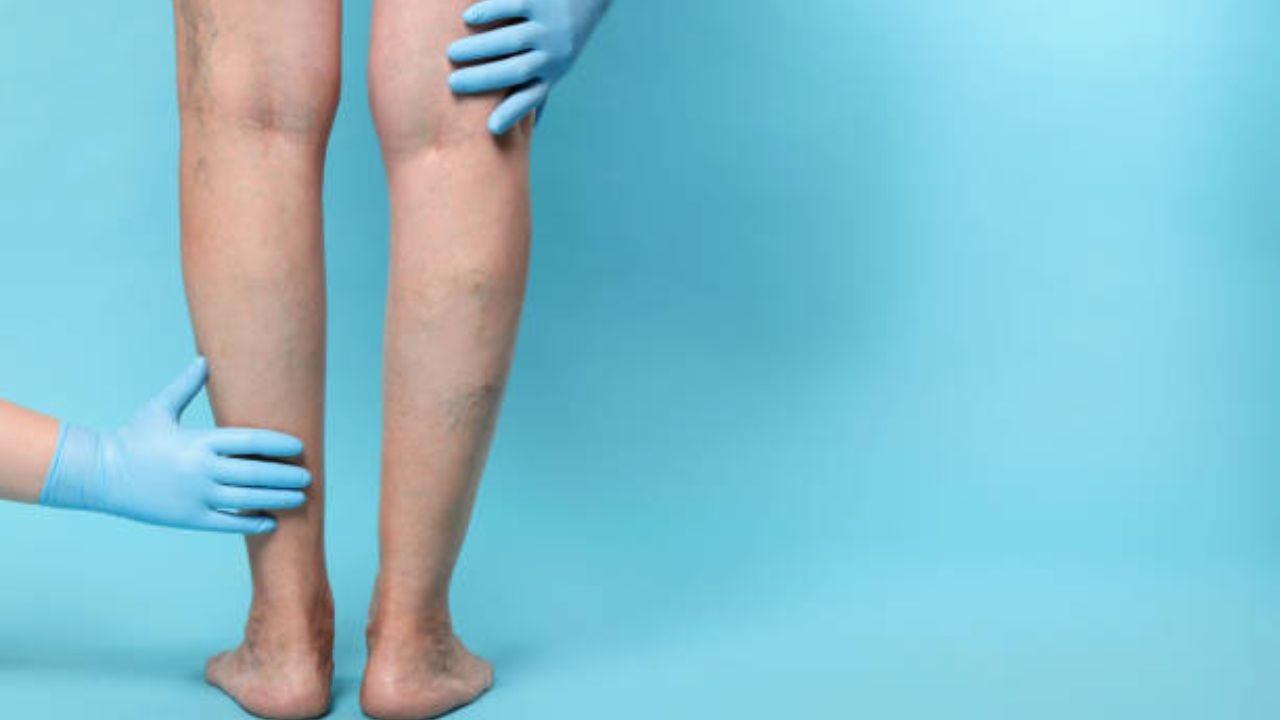
CVI doesn’t happen overnight-it develops slowly, often without anyone noticing at first. Here’s how it usually progresses:
- Valve weakening: Age, genetics, pregnancy, or long hours of standing or sitting can slowly wear down the vein valves. Yup, even small daily habits can add up over time.
- Blood pooling: Once the valves stop working efficiently, blood begins to pool in the lower legs, causing pressure to build up inside the veins.
Veins bulging: Increased pressure can make veins bulge and twist, forming what we know as varicose veins. They may look unsightly and can sometimes feel tender or achy. - Swelling and fluid buildup: Extra pressure pushes fluid into surrounding tissues, causing edema. You might notice your ankles or calves swelling by the end of the day, or shoes feeling tighter than usual.
- Skin changes and ulcers: If left untreated, CVI can lead to skin discoloration, thickening, or even venous ulcers, particularly near the ankles. These can be painful and take a long time to heal.
It’s important to know that CVI is more common than most people realize. Studies suggest that up to 40% of adults in the U.S. show some signs of chronic venous disease, and about 6-7% may develop more serious symptoms, including ulcers. Early detection is key it can help reduce discomfort, prevent serious complications, and keep your legs healthy and mobile.
Remember, your legs are trying to tell you something. Swelling, heaviness, or bulging veins aren’t just cosmetic-they’re signals that your circulatory system may need a little attention. With the right combination of lifestyle habits, medical guidance, and preventive care, you can manage CVI effectively and keep your legs feeling good for years to come.
Treatment and Lifestyle Measures
Lifestyle changes are the first step in managing CVI. Walking regularly engages calf muscles, helping blood flow back to the heart. Elevating legs after sitting or standing reduces swelling, and maintaining a healthy weight lowers vein pressure.
Compression stockings are highly effective for people at higher risk-pregnant women, those with physically demanding jobs, or anyone with visible varicose veins. They help prevent blood from pooling and reduce discomfort.
For more persistent symptoms, minimally invasive procedures such as endovenous laser therapy (EVLT) or sclerotherapy are excellent options. Laser therapy closes the damaged vein, rerouting blood through healthier veins. Recovery is generally quick, and most patients notice significant relief soon after treatment.
It’s important to know who treats venous insufficiency. Vascular specialists, interventional radiologists, and vein experts can evaluate vein function, provide treatment, and guide preventive care to avoid complications.
Expert Guidance: Keeping Veins Healthy
Managing chronic venous insufficiency successfully often requires professional guidance. Experts assess vein health through specialized imaging and physical exams, detecting problems early before they worsen. This is key because untreated CVI can progress to painful swelling, skin changes, ulcers, or even rare risks like deep vein thrombosis (DVT).
Expert guidance goes beyond procedures. Specialists advise on exercise routines, leg elevation techniques, proper compression levels, and lifestyle adjustments that reduce stress on the veins. They create personalized treatment plans, combining medical interventions with preventive care, ensuring patients experience both immediate relief and long-term improvement.
For trusted, patient-focused care, experts like Dr. Rema Malik emphasize early detection, combining lifestyle guidance with minimally invasive treatments to manage CVI effectively. With consistent follow-up, patients can reduce swelling, prevent ulcers, maintain mobility, and enjoy healthier legs for years.
Proper expert care not only addresses symptoms but also empowers patients to take proactive steps, improving quality of life, confidence, and daily comfort.
Can Chronic Venous Insufficiency Be Fatal?
Can Chronic Venous Insufficiency Be Fatal? No! Chronic venous insufficiency (CVI) itself is rarely fatal. Most people who have CVI can manage the condition safely with proper care and lifestyle adjustments. It’s important to remember that CVI is more of a long-term vein health issue than a life-threatening disease. That said, leaving CVI untreated can lead to complications that could become serious if ignored.
Over time, poorly managed CVI can cause problems such as:
- Venous ulcers: These are slow-healing, often painful sores that appear around the ankles. Because the skin and tissues are already weakened by chronic venous pressure, these ulcers can take weeks or even months to heal without proper treatment.
- Infections: Open or untreated ulcers are prone to infection. In some cases, infections can spread and become serious, requiring aggressive medical care.
- Deep vein thrombosis (DVT): Though rare, severe CVI may be associated with DVT, where a blood clot forms in a deep vein. If the clot travels to the lungs, it can cause a pulmonary embolism, a potentially life-threatening condition.
The good news is that early recognition and intervention make a huge difference. By paying attention to early signs like leg swelling, heaviness, fatigue, varicose veins, or skin changes, you can take steps to prevent severe complications.
Treatment options that help keep CVI under control include:
- Lifestyle changes: Walking, elevating the legs, maintaining a healthy weight, and avoiding prolonged sitting or standing.
- Compression therapy: Stockings or socks that improve circulation and prevent blood from pooling in the lower legs.
- Minimally invasive procedures: Techniques like endovenous laser therapy (EVLT) or sclerotherapy can close damaged veins, redirecting blood through healthier veins and providing symptom relief.
With the right care, patients can significantly reduce their risk of serious complications, improve comfort, and maintain mobility. CVI doesn’t have to control your life. Understanding the condition, staying proactive, and seeking expert guidance ensure your legs stay healthy, pain-free, and active for years to come.
Frequently Asked Questions (FAQ)
Is chronic venous insufficiency lethal?
CVI itself is rarely lethal. Serious complications like DVT or infection are uncommon, and proper care prevents most risks.
What are the early signs of CVI?
Swelling, heaviness, visible varicose veins, and skin changes around the ankles are common early indicators.
Does laser therapy work for varicose veins?
Yes. Laser therapy closes diseased veins, redirects blood through healthier veins, and usually provides fast relief with minimal downtime.
Who should I see for venous insufficiency?
Vascular specialists, interventional radiologists, or vein experts can evaluate and treat CVI effectively. Early consultation prevents complications.
References
- Society for Vascular Surgery – Chronic Venous Disease Guidelines
- American Venous Forum -Vein Health and Treatment Recommendations
- National Institutes of Health (NIH) -Chronic Venous Insufficiency Overview
- Cleveland Clinic – Varicose Veins and Venous Disorders
- Mayo Clinic – Chronic Venous Insufficiency: Causes, Symptoms, and Treatment
- Johns Hopkins Medicine – Circulatory and Vein Health
- MedlinePlus (U.S. National Library of Medicine) – Venous Disorders
- American College of Phlebology – Diagnosis and Management
- UpToDate – Chronic Venous Insufficiency: Pathophysiology and Clinical Management
European Society for Vascular Surgery – Clinical Practice Guidelines