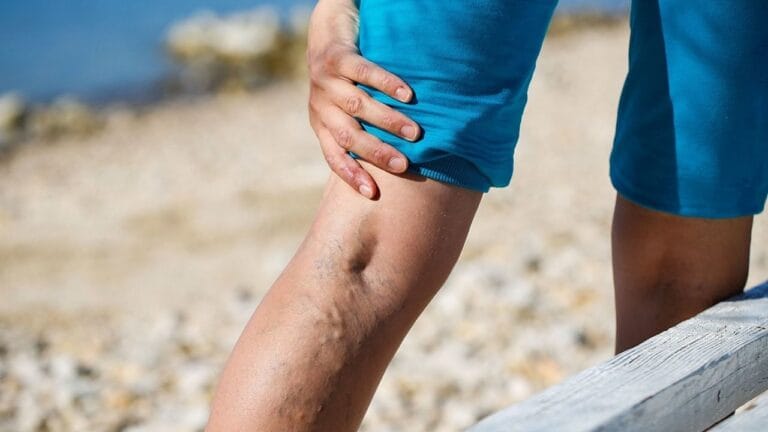
Varicose veins in individuals with obesity develop as a result of long-term strain on the venous system caused by excess body weight and reduced mobility. The increased load on the lower limbs, combined with higher intra-abdominal pressure, disrupts normal blood flow from the legs back to the heart.
Over time, this leads to weakened vein walls, valve dysfunction, and progressive venous dilation. Obesity also contributes to poor circulation and increased venous pressure, making the condition more likely to develop and progress with time.
So let’s see the details of the relation between varicose veins and obesity-
Pathophysiological Link Between Obesity and Venous Insufficiency
Obesity contributes to varicose vein formation through multiple overlapping mechanisms that affect both venous return and vascular integrity. Increased body mass, particularly central (abdominal) obesity, elevates intra-abdominal pressure. This pressure directly impedes venous return from the lower extremities through the iliac veins and inferior vena cava. As a result, venous drainage becomes inefficient, leading to chronic venous hypertension.
At the same time, prolonged venous hypertension causes:
- Distension of superficial veins.
- Progressive valve incompetence.
- Structural remodeling of venous walls.
This cycle gradually leads to visible varicosities and chronic venous disease progression.
Does Excess Weight Cause Varicose Veins?
Excess body weight is not a single direct cause but a major predisposing and accelerating factor. Obesity increases hydrostatic pressure within lower limb veins due to continuous mechanical load.
This pressure overload leads to valve stress and eventual valvular failure. Additionally, reduced mobility in obese individuals decreases the efficiency of the calf muscle pump, which is essential for venous return.
Other contributing factors include:
- Reduced venous flow velocity.
- Endothelial dysfunction.
- Increased venous wall inflammation.
- Higher risk of venous stasis.
These combined mechanisms significantly increase the likelihood of varicose vein development and progression.
Role of Venous Hypertension in Obese Individuals!
Venous hypertension is the central pathological mechanism linking obesity and varicose veins. In obese individuals, elevated intra-abdominal and lower limb pressure creates a sustained backpressure in superficial veins. This persistent pressure causes:
- Valve leaflet separation
- Reflux of blood within venous channels
- Progressive dilation of superficial veins
Over time, this leads to irreversible venous remodeling and chronic insufficiency.
Will Weight Reduction Improve Varicose Veins?
Weight reduction has a clinically significant impact on symptom relief and disease progression control. Losing weight reduces intra-abdominal pressure and improves venous return dynamics. As mechanical load decreases, venous pressure in the lower limbs reduces, allowing partial restoration of venous function.
Clinically observed improvements include:
- Reduction in leg heaviness and fatigue.
- Decrease in edema and fluid retention.
- Improved exercise tolerance.
- Slower progression of venous dilation.
However, structural venous damage such as valve incompetence and large tortuous veins may not fully reverse with weight loss alone, especially in advanced disease stages.
Varicose Veins Weight Loss: Clinical Expectations!
Weight loss plays a supportive rather than curative role in venous disease management. The benefits of weight reduction are primarily functional rather than anatomical. While symptoms improve significantly, established varicose veins may persist due to permanent connective tissue remodeling.
Key outcomes:
- Symptom improvement is often noticeable within weeks to months.
- Disease progression slows significantly.
- Recurrence risk after treatment is reduced.
- Better response to compression therapy and interventions.
Thus, weight management is considered a core component of long-term venous disease control.
Clinical Manifestations in Obesity-Related Venous Disease:
Clinical Manifestations in Obesity-Related Venous Disease (Varicose Veins Symptoms). Whatever, in obese patients, varicose vein symptoms tend to present earlier, progress faster, and persist for longer durations due to continuous venous hypertension and impaired circulation.
The increased mechanical load on the lower limb veins, combined with reduced mobility and inefficient calf muscle pump activity, creates a chronic environment of blood pooling and venous stress.
As a result, symptoms are often not just cosmetic but also functional, significantly affecting daily activity, endurance, and quality of life.
Early clinical indicators:
- Persistent heaviness in lower limbs.
- Early fatigue on standing or walking.
- Mild ankle edema.
Progressive features:
- Prominent superficial vein dilation.
- Increasing lower limb swelling.
- Burning or aching sensations.
Advanced disease:
- Chronic skin pigmentation changes.
- Venous eczema or lipodermatosclerosis.
- Recurrent nocturnal cramps.
- Risk of venous ulceration.
Preventive Strategies in Obesity-Associated Varicose Veins:
Prevention of obesity-related varicose veins is primarily aimed at reducing sustained venous pressure, improving blood circulation in the lower limbs, and enhancing the efficiency of the calf muscle pump.
Since obesity creates both mechanical and metabolic stress on the venous system, preventive strategies must be consistent, long-term, and integrated into daily lifestyle habits. Early intervention is especially important to slow disease progression and reduce the risk of chronic venous insufficiency.
1. Weight Optimization
Gradual and sustained weight reduction is one of the most effective preventive strategies. Excess body weight increases intra-abdominal pressure and venous load, so even modest weight loss can significantly improve venous return and reduce symptoms. A balanced diet combined with regular physical activity helps decrease strain on lower limb veins and supports long-term vascular health.
2. Activation of Calf Muscle Pump
Regular movement is essential for maintaining healthy venous circulation. The calf muscles act as a natural pump that pushes blood back toward the heart. Activities such as walking, light jogging, and lower limb strengthening exercises help prevent blood stagnation and reduce venous pressure. Avoiding prolonged immobility is equally important in prevention.
3. Compression Therapy
Compression stockings play a key role in maintaining proper pressure gradients within the leg veins. They help prevent blood pooling, reduce swelling, and support weakened vein walls. In obese individuals, compression therapy is often recommended as both a preventive and supportive measure to reduce symptom progression.
4. Postural and Behavioral Modification
Lifestyle adjustments are crucial in reducing venous stress. Avoiding prolonged sitting or standing without movement helps maintain active circulation. Regular position changes, short walking breaks, and elevating the legs during rest can significantly reduce venous congestion and discomfort.
5. Hydration and Circulatory Support
Adequate hydration supports overall blood flow and reduces blood viscosity, which can improve circulation efficiency. Combined with light physical activity, proper hydration helps maintain healthier vascular function and reduces the risk of venous stagnation.
6. Long-Term Activity Planning
In obese individuals, structured daily routines that include consistent movement, exercise, and rest intervals are essential. Even small but regular physical activity throughout the day is more effective than occasional intense exercise, as it continuously supports venous return and reduces pressure buildup.
Overall, preventive strategies work best when combined, rather than used individually, forming a comprehensive approach to managing obesity-associated varicose veins and slowing disease progression.
Treatment Approach in Obesity-Related Varicose Veins
Management of varicose veins treatment in obese individuals is typically multimodal, progressive, and stage-dependent, meaning treatment is selected based on the severity of venous disease, symptom burden, and overall patient health status.
Because obesity itself is a contributing factor, effective management requires both symptom control and correction of underlying risk factors to achieve long-term improvement.
In the early stages, treatment mainly focuses on conservative strategies aimed at improving venous return and reducing venous pressure.
As the condition progresses, a combination of conservative and interventional approaches may be required to prevent complications such as chronic venous insufficiency, skin changes, and ulcer formation.
Conservative management:
- Weight reduction programs.
- Exercise therapy.
- Compression stockings.
- Lifestyle modification.
Interventional management:
In cases of advanced venous insufficiency:
- Endovenous laser therapy (EVLT).
- Minimally invasive ablation techniques.
These are often more effective when combined with weight control strategies.
When Specialist Evaluation Is Required?
Specialist consultation becomes essential when venous disease progresses beyond simple discomfort and begins to affect daily function, skin integrity, or overall quality of life.
In obesity-related varicose veins, early progression can sometimes be subtle, but underlying venous hypertension may already be advancing.
Timely evaluation by a vascular specialist helps in accurate staging of the disease, identifying complications, and selecting the most appropriate treatment plan before irreversible changes occur.
Clinical indications include:
- Persistent lower limb pain despite conservative care.
- Progressive vein enlargement.
- Skin discoloration or hardening.
- Recurrent swelling not improving with rest.
- Signs of chronic venous insufficiency.
Early vascular evaluation allows staging of disease and prevention of long-term complications. For expert diagnosis, staging, and personalized treatment planning, consultation with Dr. Ream Malik is recommended.
Conclusion
Obesity significantly contributes to the development and progression of varicose veins through sustained venous hypertension, impaired muscle pump function, and vascular remodeling. While weight loss alone may not reverse established venous damage, it remains one of the most important factors in symptom control and disease stabilization.
A combined approach involving weight management, compression therapy, and early clinical intervention provides the most effective long-term outcomes in obesity-associated venous disease.
References
- American College of Phlebology. (2022). Chronic venous disease: Clinical guidelines and management. https://www.phlebology.org
- Bergan, J. J., Schmid-Schönbein, G. W., Smith, P. D., Nicolaides, A. N., Boisseau, M. R., & Eklof, B. (2006). Chronic venous disease. New England Journal of Medicine, 355(5), 488–498. https://doi.org/10.1056/NEJMra055289
- Eberhardt, R. T., & Raffetto, J. D. (2014). Chronic venous insufficiency. Circulation, 130(4), 333–346. https://doi.org/10.1161/CIRCULATIONAHA.113.006898
- Kahn, S. R., Shrier, I., Kearon, C., et al. (2011). Determinants and time course of the postthrombotic syndrome after deep venous thrombosis. Annals of Internal Medicine, 149(10), 698–707. https://doi.org/10.7326/0003-4819-149-10-200811180-00005
- Lurie, F., Passman, M., Meisner, M., et al. (2020). The 2020 update of the guidelines for management of chronic venous disease. Journal of Vascular Surgery: Venous and Lymphatic Disorders, 8(1), 1–24. https://doi.org/10.1016/j.jvsv.2019.09.006
- National Institute for Health and Care Excellence (NICE). (2013). Varicose veins in the legs: Diagnosis and management (CG168). https://www.nice.org.uk/guidance/cg168
- Nicolaides, A. N. (2012). Investigation of chronic venous insufficiency: A consensus statement. Circulation, 126(4), 575–580. https://doi.org/10.1161/CIRCULATIONAHA.112.096230
- O’Donnell, T. F., Passman, M. A., Marston, W. A., et al. (2014). Management of venous leg ulcers: Clinical practice guidelines. Journal of Vascular Surgery, 60(2 Suppl), 3S–59S. https://doi.org/10.1016/j.jvs.2014.04.049
- Society for Vascular Surgery. (2022). Clinical practice guidelines on venous disease. https://vascular.org
- UpToDate. (2024). Chronic venous disease and varicose veins in adults. Wolters Kluwer. https://www.uptodate.com