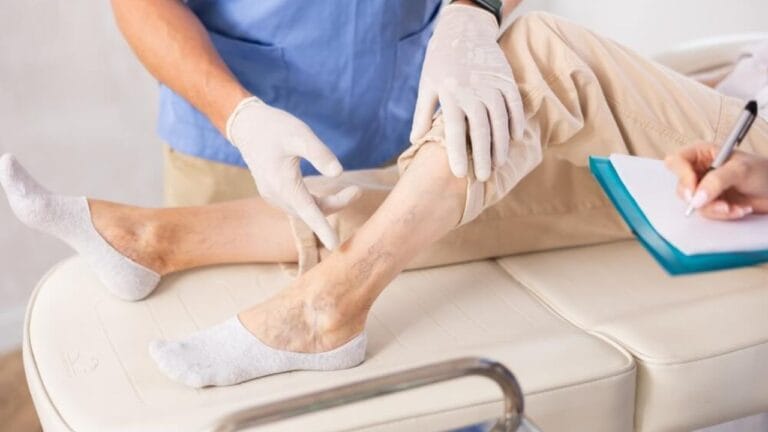
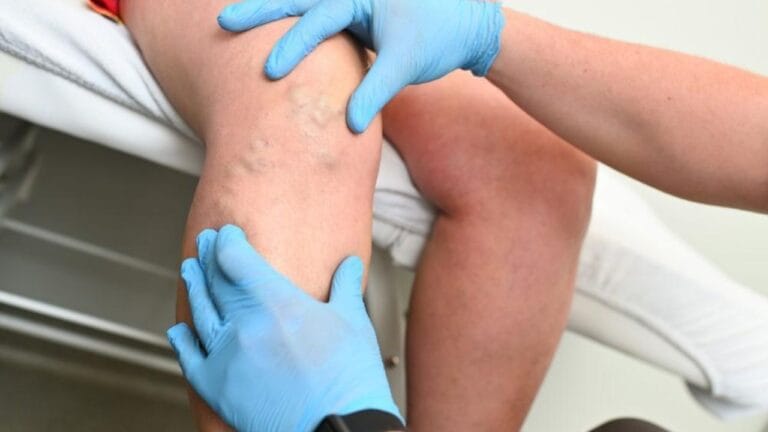
Chronic venous insufficiency (CVI) is a silent but serious condition that affects millions of adults worldwide. It starts with tired, heavy legs and swelling, but can quietly progress to skin damage, ulcers, and mobility issues if ignored. Understanding the risks and taking early action is essential to protect your legs, improve circulation, and maintain a better quality of life.
However, let’s see a detailed session on how dangerous chronic venous insufficiency can be. In this article, we’ll break down how dangerous CVI can be, explore the factors that increase its risks, and explain the steps you can take to manage it effectively.
Let’s go into the details-
How Dangerous Is Chronic Venous Insufficiency?
Chronic venous insufficiency (CVI) is far more than a cosmetic issue or minor leg discomfort. It is a progressive vascular condition in which the veins, particularly in the legs, fail to return blood efficiently to the heart. When blood pools in the lower limbs, pressure builds in the veins, damaging the vein walls and valves over time. This results in swelling, leg heaviness, varicose veins, skin discoloration, and, in severe cases, painful ulcers.
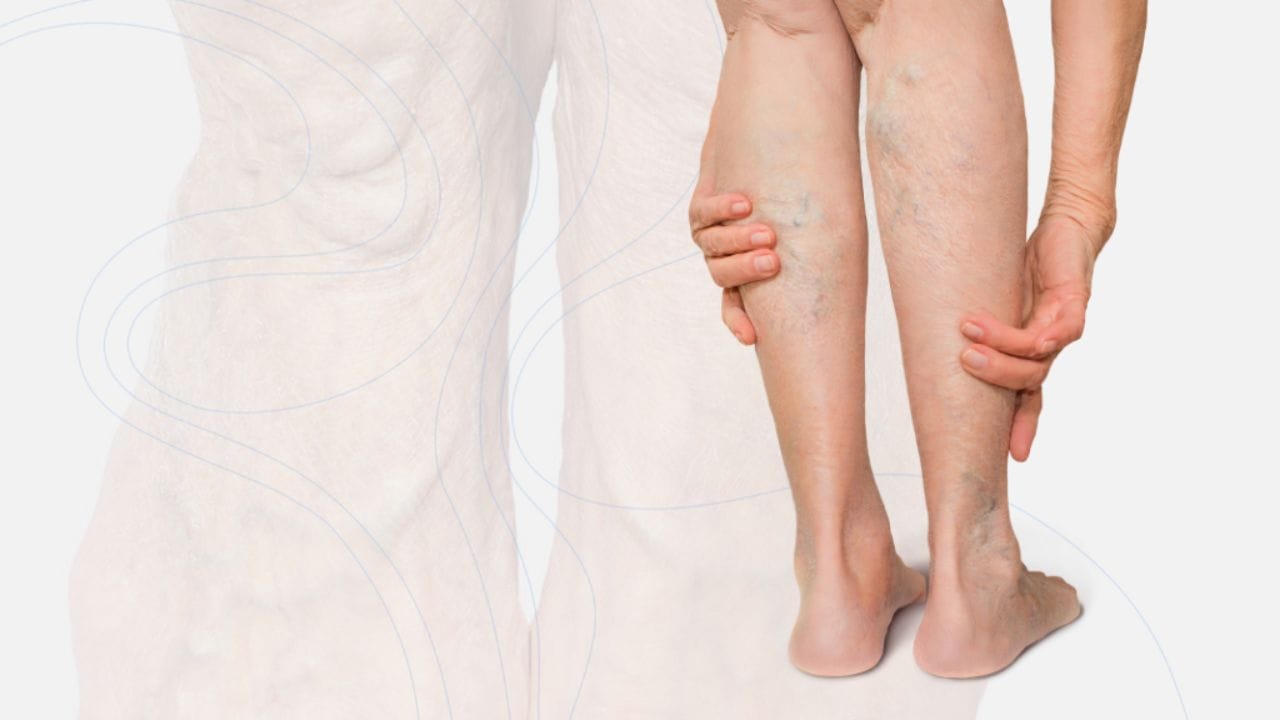
CVI can develop silently and worsen gradually, meaning many patients are unaware of the severity of their condition until serious complications arise. Understanding the dangers of CVI and how to prevent its progression is crucial for maintaining long-term vascular health.
“Chronic venous insufficiency is heavily influenced by lifestyle. Small changes like moving regularly, maintaining a healthy weight, and avoiding long periods of standing can significantly reduce symptom progression and improve quality of life.”
— Vascular Specialist (based on clinical guidelines)
Prevalence and Demographics
Chronic venous insufficiency is a common condition affecting millions worldwide. According to epidemiological studies:
- 20-40% of adults globally show signs of venous insufficiency, with prevalence increasing with age.
- Women are affected more frequently than men, with some studies showing up to 40% of adult women experience CVI symptoms, compared to 1-17% of men.
- Severity also correlates with age: adults over 65 are at the highest risk of developing advanced disease, including skin changes and venous ulcers.
The high prevalence emphasizes the importance of early detection and lifestyle modifications to prevent long-term complications.
Factors That Make Chronic Venous Insufficiency Dangerous
- Age
As we age, vein walls weaken, and the valves that prevent blood from flowing backward become less efficient. This can cause blood to pool in the legs, leading to chronic swelling, skin changes, and even painful ulcers. Studies show that over 50% of adults above 50 may exhibit signs of CVI, highlighting the importance of early monitoring. - Genetics
A family history of venous disease significantly increases the risk of CVI. Inherited factors can affect vein elasticity and valve strength, making some individuals more vulnerable to complications even if they maintain a healthy lifestyle. - History of Deep Vein Thrombosis (DVT)
DVT can cause permanent valve damage in the veins. Up to 50% of DVT patients may develop post-thrombotic syndrome, a severe form of CVI, which increases the likelihood of chronic pain, swelling, and ulcers over time. - Obesity
Excess body weight increases pressure in the leg veins and reduces effective blood flow back to the heart. Obese individuals are 2–3 times more likely to develop advanced CVI, with higher risks of persistent swelling, skin changes, and slow-healing ulcers. - Prolonged Standing or Sitting
Extended periods of standing or sitting without movement elevate venous pressure and strain the valves. Jobs that require long hours of standing or sitting, like retail, teaching, or desk work, can accelerate varicose veins, leg heaviness, and swelling. Regular movement and leg elevation are key preventive steps.
How CVI Progresses and Why It’s Dangerous
1. Venous Leg Ulcers
Venous leg ulcers are the most severe and dangerous complication of CVI. They occur when chronic venous pressure damages the skin and surrounding tissues. Up to 3% of adults may develop venous ulcers in their lifetime. Healing is slow, and recurrence rates are high, ranging from 40% to 80%, depending on adherence to compression therapy.
Ulcers significantly affect mobility, productivity, and quality of life, and can lead to infections if not managed properly. If you’re also concerned about appearance, check out Is It Too Late To Get Cosmetic Vein Treatment? to learn about combining medical care with aesthetic treatments.
2. Skin Changes and Infections
Chronic swelling can make the skin fragile, dry, and discolored. Lipodermatosclerosis—a hardening of the skin and fat—may develop, making minor injuries prone to infection. Cellulitis is a frequent complication, sometimes requiring hospitalization.
For patients concerned about spider veins or visible varicose veins, Best Cosmetic Procedures To Treat Spider Veins explains medical and cosmetic options that complement CVI management.
3. Risk of Deep Vein Thrombosis (DVT)
Blood pooling in weakened veins can lead to clot formation. DVT is dangerous because if a clot breaks free, it may travel to the lungs and cause a pulmonary embolism, a potentially fatal event.
4. Chronic Pain and Reduced Mobility
CVI leads to leg heaviness, fatigue, and intermittent cramps, limiting mobility. Reduced movement worsens venous return and accelerates disease progression.
Impact on Quality of Life
CVI significantly affects daily life:
- Up to 90% of patients report chronic pain, discomfort, or leg swelling.
- Sleep disturbances from nighttime cramps are common.
- Emotional impacts include anxiety, depression, and social withdrawal.
- Economic impacts include lost workdays, reduced productivity, and ongoing medical costs.
These factors make CVI a public health concern, not just a cosmetic or minor vascular issue.
Management and Prevention
While CVI cannot always be reversed, proper management can slow progression, prevent complications, and improve quality of life.
Lifestyle Modifications
- Daily walking or calf exercises to improve venous return.
- Avoid prolonged sitting or standing; elevate legs during rest.
- Maintain a healthy weight to reduce venous pressure.
Medical Interventions
- Compression therapy: Medical-grade stockings reduce edema, improve circulation, and prevent ulcers.
- Minimally invasive procedures: Laser or radiofrequency ablation, sclerotherapy for varicose veins.
- Surgery: Reserved for severe cases with structural vein abnormalities.
“Early diagnosis and intervention are the most effective ways to reduce the dangers of chronic venous insufficiency. Patients who follow lifestyle changes and therapy regimens see dramatic improvements in symptoms and long-term outcomes.”
— Vascular Specialist
However, for personalized evaluation and treatment options, you can consult Dr. Rema Malik, an expert in vascular health and venous disease management. She can assess your condition, recommend the most suitable therapies, and guide you on lifestyle changes to prevent complications. Early intervention can significantly improve your quality of life and reduce the risk of severe venous issues.
Severity and Risk Table (CEAP Classification)
| CEAP Category | Clinical Features | Risk Level |
| C1-C2 (Mild) | Spider veins, minor varicose veins | Low |
| C3-C4 (Moderate) | Persistent edema, skin changes, pigmentation | Moderate |
| C5-C6 (Severe) | Healed or active venous ulcers | High |
This table helps both patients and clinicians understand the stage of CVI and associated risks.
Conclusion
Chronic venous insufficiency is a serious, progressive condition that poses risks beyond cosmetic concerns. If left untreated, it can lead to ulcers, infections, DVT, chronic pain, and a significant reduction in quality of life.
Early recognition, lifestyle modifications, compression therapy, and timely medical intervention are critical to prevent severe outcomes. Patients should monitor for symptoms like swelling, skin changes, or persistent leg discomfort and seek professional evaluation promptly.
Take control of your venous health today-don’t wait until complications arise. Small changes can make a big difference in your long-term mobility and quality of life.