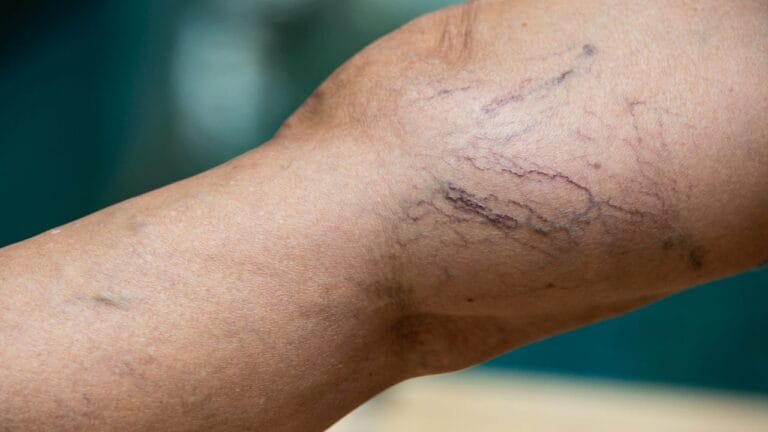
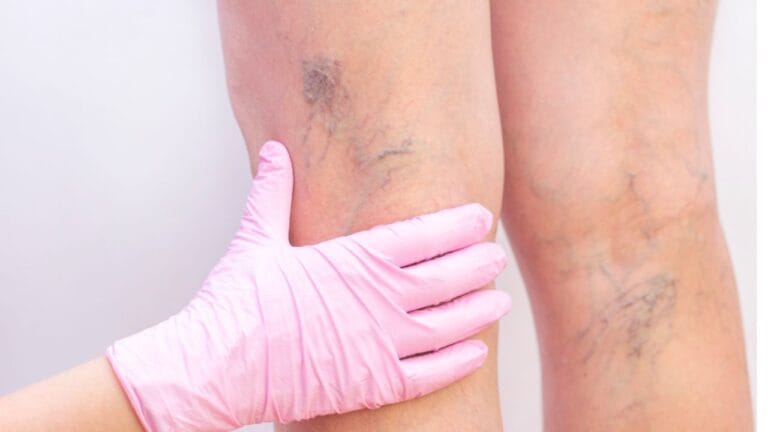
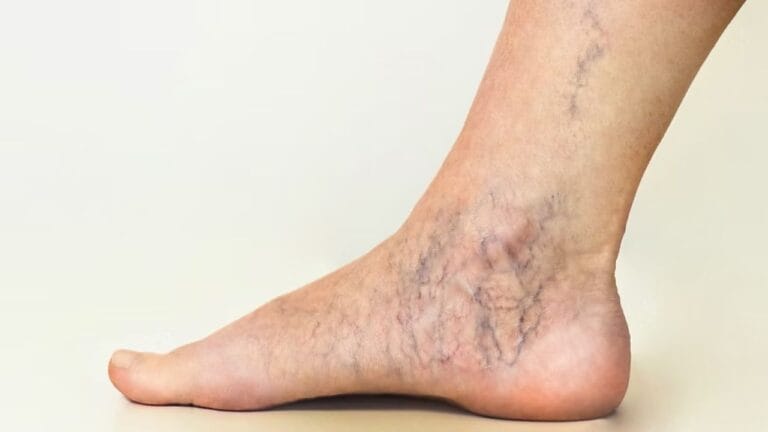
Varicose veins are more than a cosmetic concern-they are often a visible sign of underlying venous disease. Understanding the stages of varicose veins is crucial because early detection can prevent progression into more serious conditions like chronic venous insufficiency (CVI).
Medical professionals rely on structured systems such as the CEAP classification and the varicose veins severity scale to evaluate how far the disease has progressed and what kind of treatment is needed.
Let see the details-
What Are Varicose Veins and Why Do They Progress?
Varicose veins develop when the valves inside your veins weaken or become damaged. These valves are responsible for keeping blood flowing upward toward the heart. When they fail, blood starts pooling in the veins, especially in the legs, causing them to enlarge, twist, and become visible. Over time, this condition can worsen due to factors like aging, prolonged standing, obesity, pregnancy, and genetics.
According to the National Institutes of Health, chronic venous disorders affect nearly 25-30% of adults, with a higher prevalence among women.
Varicose Veins Stages: The Clinical Progression (CEAP Classification Explained in Detail)
Doctors worldwide rely on the CEAP classification (Clinical, Etiological, Anatomical, Pathophysiological) to accurately assess the progression of varicose veins. This system doesn’t just describe how veins look-it helps determine how serious the underlying venous disease has become.
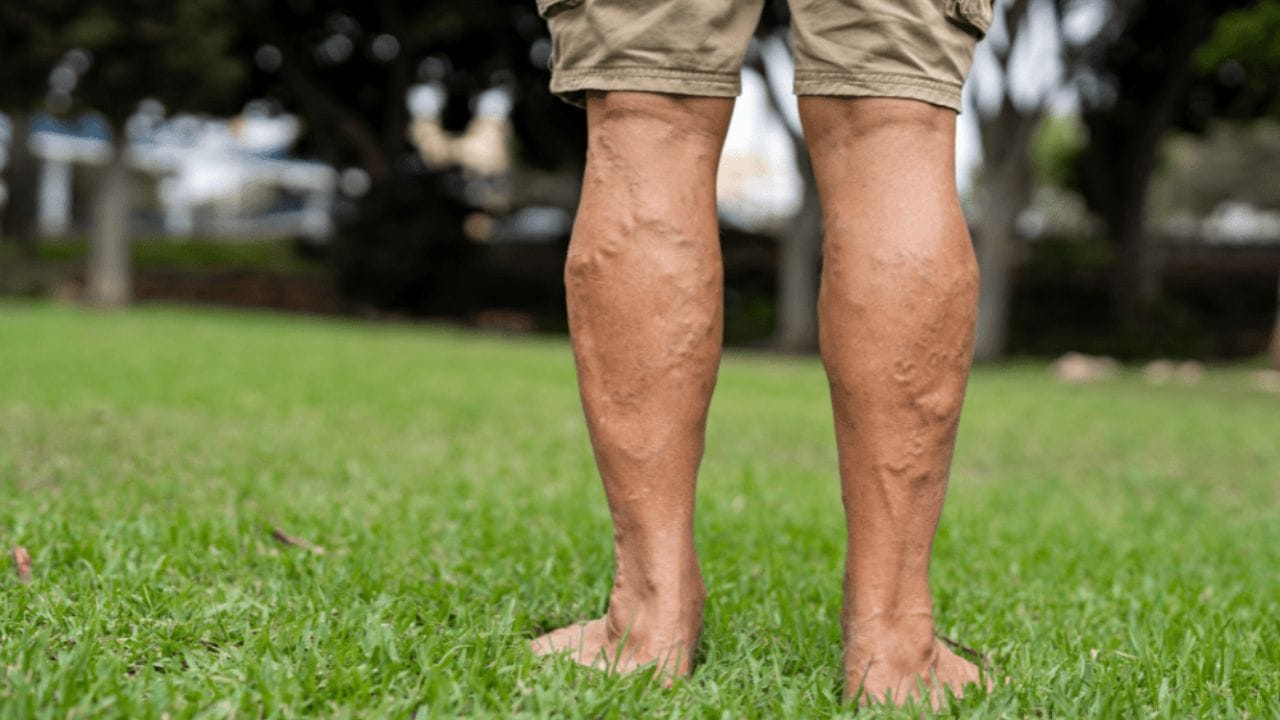
Below is a more detailed, clinically grounded breakdown of each stage, so you can clearly understand how the condition progresses over time.
Stage C0: No Visible Signs (Early Functional Changes)
At this stage, there are no visible veins, which is why many people ignore the symptoms. However, your veins may already be struggling internally.
You may notice:
- A heavy or tired feeling in your legs
- Mild aching after long periods of standing
- Occasional discomfort without visible cause
This stage is often called a “silent phase,” where venous dysfunction begins but hasn’t yet appeared externally.
Stage C1: Spider Veins (Telangiectasia)
At this stage, small red, blue, or purple veins become visible on the surface of your skin. These are known as spider veins.
Although usually painless, they indicate:
- Early weakening of vein walls
- Initial failure of small blood vessels
- Beginning of circulation imbalance
Many people consider this a cosmetic issue, but medically, it signals the first visible stage of venous disease.
Stage C2: True Varicose Veins (Visible Vein Enlargement)
Now the condition becomes clearly noticeable and medically significant.
You may experience:
- Bulging, twisted veins (often dark blue or purple)
- Throbbing or aching pain
- Heaviness that worsens throughout the day
- Mild swelling in legs or ankles
At this stage, blood is no longer flowing efficiently upward. Instead, it pools in the veins, increasing pressure.
According to Dr. Rema Malik,
“By the time veins become visibly enlarged, the underlying valve dysfunction is already well established and requires clinical attention.”
Stage C3: Edema (Persistent Swelling)
At Stage C3, swelling becomes more noticeable and frequent. Key signs include:
- Swelling in the ankles and lower legs.
- Tightness in the skin.
- Symptoms worsen by evening and improve after rest.
This happens because fluid leaks from the veins into the surrounding tissues due to increased pressure. Clinically, this stage indicates that the condition is no longer superficial—it is affecting circulatory efficiency.
Stage C4: Skin Changes (Chronic Damage Begins)
At this stage, long-term poor circulation begins to damage the skin. You may notice:
- Darkening of the skin (hyperpigmentation).
- Itching, dryness, or eczema-like irritation.
- Thickened, hardened skin (lipodermatosclerosis).
These changes occur because oxygen and nutrients are not properly reaching the skin. As specialists explain, “Skin changes are often the turning point where venous disease shifts from manageable to potentially chronic if untreated.”
Stage C5: Healed Venous Ulcers
At this stage, open wounds (ulcers) have already formed but have healed. However:
- The skin remains fragile.
- Circulation is still compromised.
- There is a high risk of recurrence.
This stage indicates a history of severe venous disease, even if the skin looks temporarily better.
Stage C6: Active Venous Ulcers (Most Severe Stage)
This is the most advanced and serious stage of varicose veins.
Characteristics include:
- Open, non-healing wounds (usually near the ankles).
- Pain, tenderness, and swelling.
- Risk of infection and complications.
These ulcers develop due to prolonged high pressure in the veins, which damages the surrounding tissue. Clinical data suggest that venous ulcers affect 1-3% of adults globally, and healing can take weeks to months without proper treatment.
Each stage represents a progressive worsening of venous function. What starts as mild discomfort (C0-C1) can eventually lead to chronic wounds (C5-C6) if left untreated. The earlier you recognize symptoms, the easier it is to: Prevent complications, avoid invasive treatments, and maintain long-term leg health.
Varicose Veins Severity Scale: How Doctors Measure Progression?
Beyond visual staging, clinicians also use the Venous Clinical Severity Score (VCSS) to quantify disease severity. This scale evaluates: Pain level, Degree of swelling, Skin changes, Ulcer presence, and duration. Each factor is scored, helping doctors track progression and treatment effectiveness over time.
Mild vs Severe Varicose Veins: Key Differences
Understanding the difference between mild and severe varicose veins can help you decide when to seek medical attention.
Mild cases (C1-C2):
- Mostly cosmetic.
- Occasional discomfort.
- Minimal impact on daily life.
Severe cases (C3-C6):
- Chronic swelling.
- Skin damage.
- Risk of ulcers and infection.
- Reduced mobility and quality of life.
According to the Society for Vascular Surgery, untreated venous disease can progressively worsen in over 50% of patients if left unmanaged.
How Dangerous Is Chronic Venous Insufficiency?
How dangerous is chronic venous insufficiency ? Well, chronic venous insufficiency (CVI) is the advanced form of untreated varicose veins. It is not immediately life-threatening, but it can lead to serious complications if ignored.
Long-term CVI can cause:
- Persistent pain and swelling.
- Skin breakdown.
- Venous ulcers.
- Increased risk of infection.
A clinical review published in the Journal of Vascular Surgery notes that untreated CVI significantly impacts quality of life and may lead to long-term disability.
When to See a Professional Consultation?
Many people tend to ignore varicose veins, assuming they are only a cosmetic issue. However, this is a progressive condition that can worsen over time if left untreated. Knowing when to seek professional help can make a significant difference in preventing complications.
You should consider consulting a specialist if you notice:
- Persistent leg pain, heaviness, or discomfort.
- Swelling in the legs or ankles, especially after standing.
- Visible, bulging, or twisted veins.
- Skin discoloration or itching around the affected area.
- Thickened or hardened skin near the lower legs.
- Open wounds or sores that heal slowly.
These symptoms may indicate that your condition is progressing and could lead to more serious vascular complications if not treated properly.
If you are experiencing any of these signs, seeking care from an experienced vascular specialist like Dr. Rema Malik can help you get an accurate diagnosis and a personalized treatment plan tailored to your condition.
Early consultation not only helps manage symptoms effectively but also reduces the risk of advanced stages such as venous ulcers or chronic venous insufficiency.
Can You Die from Chronic Venous Insufficiency?
Can you die from chronic venous insufficiency? Well, it needs a little bit of detailed discussion. While CVI itself is rarely fatal, complications arising from it can become serious. In rare cases, untreated venous ulcers may become infected, leading to systemic infection (sepsis).
Additionally, venous disease may coexist with conditions like deep vein thrombosis (DVT), which can lead to pulmonary embolism, a potentially life-threatening condition. This is why early diagnosis and management are critical, even in the early stages of varicose veins.
So the gist is?
Chronic venous insufficiency (CVI) is usually not directly life-threatening, so you typically cannot die from CVI itself. However, in advanced or untreated cases, it can lead to serious complications.
Why Early Treatment Matters?
The progression from mild spider veins to severe ulcers is often gradual but preventable. Early intervention, such as compression therapy, lifestyle changes, or minimally invasive procedures, can significantly slow or even stop disease progression.
Modern treatments like endovenous laser therapy (EVLT) and radiofrequency ablation (RFA) have shown success rates of over 90%, according to multiple vascular studies.
However, for advanced care options, many patients explore professional Varicose Vein Treatment to reduce symptoms and improve circulation.
An untreated progression can lead to chronic complications that significantly impact mobility and quality of life over time. Regular follow-up with a vascular specialist is essential for long-term prevention and effective disease management.
Conclusion
Understanding the stages of varicose veins helps you recognize when a seemingly minor issue becomes a serious medical condition. From early spider veins to advanced ulcers, each stage represents a progression that can and should be managed proactively.
If you notice symptoms like swelling, visible veins, or skin changes, seeking medical evaluation early can make a significant difference in long-term outcomes.
So that’s all on the stages of varicose veins. Still you have any quetries, pls let me know –
References
- Eberhardt, R. T., & Raffetto, J. D. (2014). Chronic venous insufficiency. Circulation, 130(4), 333–346.
- Gloviczki, P., et al. (2011). The care of patients with varicose veins and associated chronic venous diseases. Journal of Vascular Surgery, 53(5), 2S–48S.
- National Institutes of Health. (2023). Venous disease statistics and prevalence.
- Society for Vascular Surgery. (2022). Clinical practice guidelines for varicose veins management.