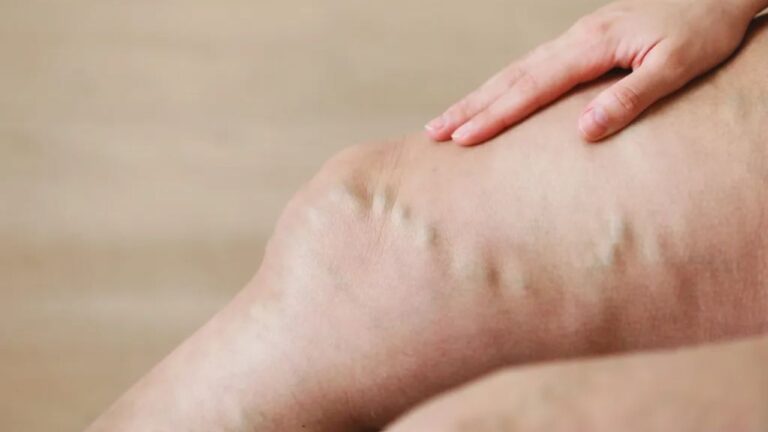
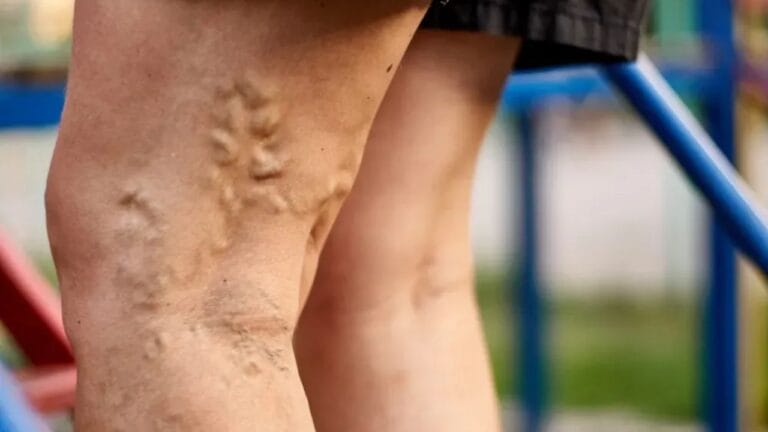
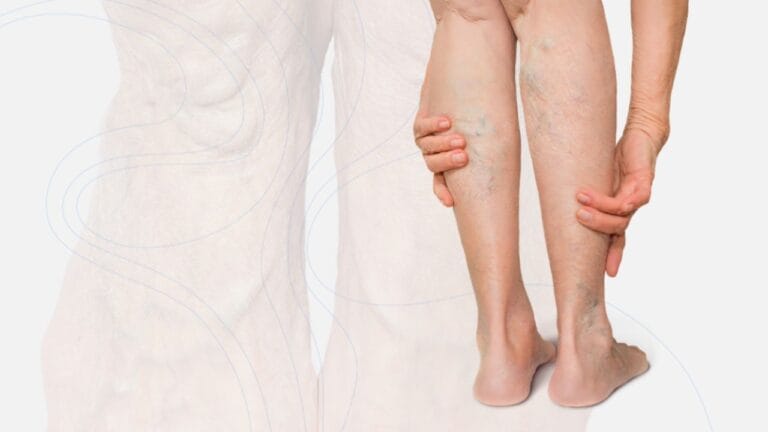
Varicose veins are a common condition where veins, usually in the legs, become enlarged, twisted, and visible under the skin. This happens when the tiny valves inside the veins stop working properly, causing blood to collect instead of flowing smoothly back to the heart.
Understanding varicose veins symptoms is important because they are not only a cosmetic issue. In many cases, they can be a sign of poor blood circulation. Finding the symptoms early can help prevent the condition from getting worse and reduce the risk of more serious problems later.
Let’s see the detailed discussion now-
Epidemiology & Clinical Significance
Varicose veins are highly prevalent across different populations, making them a significant public health concern. Studies suggest that up to one-third of adults may develop this condition at some point in their lives, with a higher incidence in aging populations.
The condition is not merely aesthetic-many patients experience discomfort, reduced mobility, and decreased quality of life. Recognizing symptom patterns helps clinicians determine disease severity and appropriate intervention strategies.
Clinical Appearance of Varicose Veins
The visual presentation of varicose veins is often the first indicator prompting patients to seek medical advice. These veins typically appear enlarged, twisted, and raised above the skin surface.
While some individuals may initially consider them a cosmetic issue, visible vein changes often reflect deeper circulatory dysfunction that requires clinical evaluation.
As the condition progresses, the affected veins may become more prominent, darker in color, and increasingly visible through the skin. In many cases, patients also notice clustering of veins or a rope-like appearance along the legs, especially after prolonged standing or physical activity.
In addition, these visible changes are frequently accompanied by symptoms such as heaviness, aching, or swelling, which further indicate impaired venous return. Early recognition of these signs is important, as timely medical assessment can help prevent progression to chronic venous insufficiency and other complications.
Varicose Veins Symptoms
The signs of varicose veins are primarily observable physical changes in the veins and surrounding skin. These signs often develop gradually and may go unnoticed in early stages.
Common visible signs include bulging veins, dark discoloration (blue or purple), and the presence of spider veins. These changes occur due to weakened vein walls and malfunctioning valves, leading to improper blood flow and venous pooling.
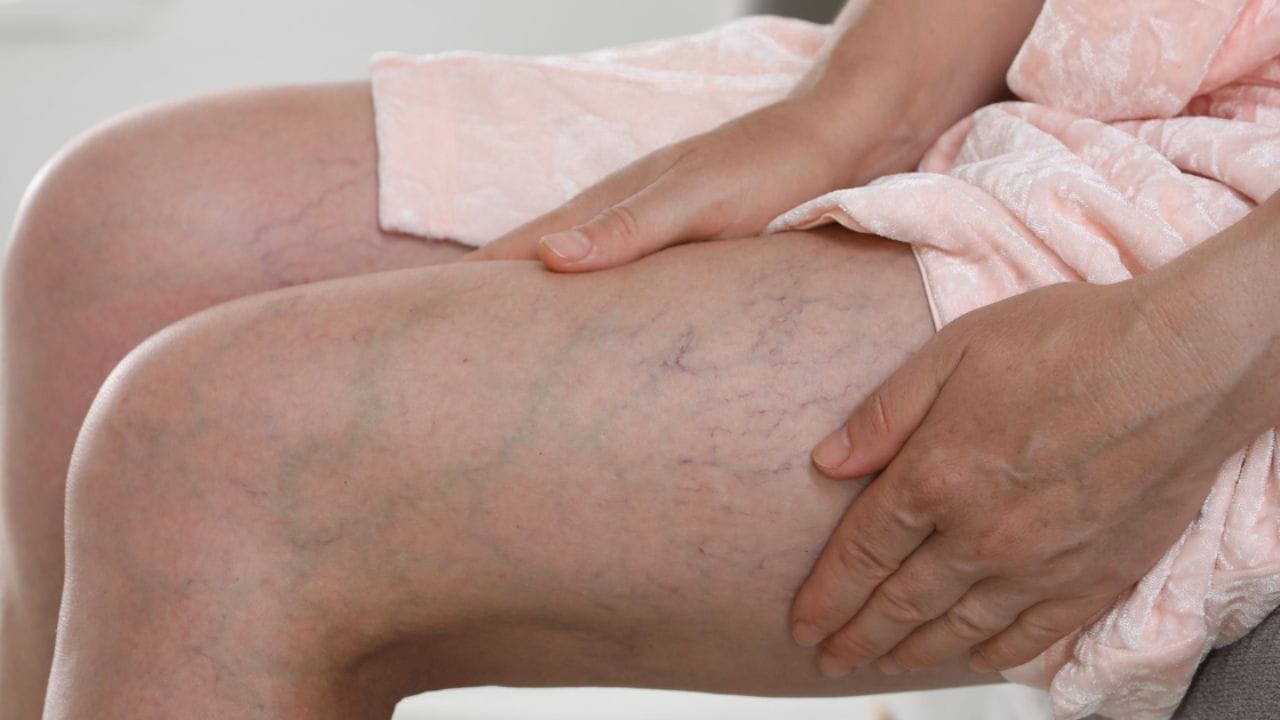
However, the varicose veins symptoms in legs are the most commonly reported, as the lower extremities are subjected to the greatest gravitational pressure. Symptoms tend to worsen after prolonged standing or sitting.
Patients frequently report heaviness, aching pain, swelling, and muscle cramps. These symptoms are often relieved by elevating the legs or engaging in physical movement, which helps improve circulation and reduce venous pressure.
Early Signs of Varicose Veins
Recognizing the early signs of varicose veins is crucial for preventing disease progression and complications. Early-stage symptoms are often subtle and may be mistaken for general fatigue or muscle strain.
These signs include mild leg heaviness, slight swelling, and occasional discomfort after prolonged standing. Increased visibility of veins beneath the skin may also appear. Early intervention at this stage can significantly slow or halt progression.
Varicose Veins Symptoms Female
Hormonal and physiological factors often influence the varicose veins symptoms that female patients experience. Women are more likely to develop varicose veins due to hormonal fluctuations and life events such as pregnancy.
Symptoms may worsen during menstrual cycles or pregnancy due to increased blood volume and hormonal effects on vein elasticity. Female patients commonly report increased swelling, discomfort, and vein prominence during these periods.
Varicose Veins Symptoms in Male Patients
In male patients, varicose veins are commonly associated with prolonged standing, physical labor, obesity, and reduced activity. Symptoms typically include visible enlarged veins, leg heaviness, aching, and fatigue that worsen after long periods of standing or walking. Ankle swelling may also occur, particularly at the end of the day.
Unlike in females, symptoms are not influenced by hormonal changes but may gradually progress over time if untreated.
Symptom Severity Classification Table
Symptom severity varies depending on the stage of the disease and underlying venous dysfunction. Early stages may present with minimal discomfort, while advanced stages can significantly impact daily activities.
The table below provides a structured overview of how symptoms progress:
| Stage | Clinical Features | Patient Experience |
| Early | Mild vein visibility, slight heaviness | Cosmetic concern |
| Moderate | Pain, swelling, cramps | Functional discomfort |
| Advanced | Skin discoloration, ulcers | Significant morbidity |
Symptom Prevalence Chart (General Trends)
Different symptoms of varicose veins occur at varying frequencies depending on patient demographics and disease progression. Understanding these trends helps clinicians prioritize diagnosis and treatment.
The following chart summarizes commonly reported symptom prevalence:
| Symptoms | Approximate Frequency |
| Visible veins | Verry common |
| Leg heaviness | Common |
| Pain/cramping | Moderate |
| Skin changes | Less common |
| Ulcers | Rare but severe |
Pathophysiology Insight
The development of varicose veins is primarily associated with venous valve incompetence and sustained elevation of venous pressure. When the valves within the superficial veins fail to function properly, blood begins to flow retrograde and pool within the affected vessels. This venous reflux increases intraluminal pressure, leading to progressive venous dilation, elongation, and tortuosity.
Over time, these hemodynamic changes contribute to the development of chronic venous insufficiency, a condition in which the venous system is unable to effectively return blood to the heart. The resulting venous hypertension triggers a cascade of structural and inflammatory changes in the vein wall and surrounding tissues.
Clinically, these underlying mechanisms manifest as lower limb swelling, aching pain, heaviness, and, in more advanced cases, skin changes such as hyperpigmentation, lipodermatosclerosis, and ulceration.
1) Valve dysfunction as a cause
In Varicose veins, venous valve failure is the primary mechanism in the vast majority of cases, well over 90%. Most varicose veins arise from superficial venous valve incompetence, leading to reflux and venous pooling.
2) How common the condition is (population percentage)
- About 10-30% of adults develop visible varicose veins at some point.
- In women, the prevalence is often higher: ~20-40% depending on age and risk factors.
- In men: typically ~10-20%.
3) Progression to chronic venous insufficiency
A smaller proportion progresses to significant disease:
- Roughly 5-15% of adults may develop clinically significant Chronic venous insufficiency with symptoms like edema, skin changes, or ulcers.
Expert Insight & Clinical Evidence
“Varicose veins are often the first visible sign of a deeper circulatory issue. Early symptoms like heaviness and fatigue should never be ignored.” – Vascular Specialist Insight shared on professional networks (LinkedIn clinical discussion)
Medical experts consistently emphasize that varicose veins are not merely a cosmetic concern but a manifestation of underlying venous insufficiency. Symptoms such as aching, swelling, and cramping often reflect compromised blood flow and increased venous pressure, which can worsen over time if left untreated.
From a clinical standpoint, research indicates a strong correlation between symptom severity and disease progression. Studies show that nearly 20-25% of individuals with varicose veins develop chronic venous insufficiency, while approximately 2-6% may progress to advanced complications such as skin changes or venous ulcers. This highlights the importance of early detection and proactive management.
Evidence-Based Insights
- Around 30% of adults worldwide are affected by varicose veins.
- Women are 2-3 times more likely to develop symptomatic disease.
- Up to 50% of patients report pain or heaviness as primary symptoms.
- Chronic venous disorders account for a significant portion of the vascular healthcare burden globally.
These statistics reinforce that symptom progression is not random-it follows a predictable clinical trajectory linked to venous dysfunction and lifestyle risk factors.
“What many patients consider minor discomfort is actually a signal of progressive venous disease. Timely intervention can prevent long-term damage.” – Endovascular physician insight (LinkedIn professional post)
Advanced Clinical Interpretation
“In my clinical experience, patients who seek treatment early have significantly better outcomes and fewer complications compared to those who delay care.” – Board-certified vein specialist (LinkedIn medical commentary)
From a pathophysiological perspective, symptom escalation is closely tied to venous hypertension and valve incompetence. As pressure builds within the veins, it leads to inflammation, tissue damage, and eventual skin changes.
Over time, this can result in:
- Lipodermatosclerosis (skin thickening).
- ● Hyperpigmentation.
- Venous ulcers in advanced stages.
These findings underscore why clinicians stress early diagnosis and structured treatment plans-not only to relieve symptoms but also to halt disease progression at its source.
When Symptoms Indicate Complications
In some cases, varicose veins can lead to serious complications if left untreated. Warning signs include persistent swelling, severe pain, and skin ulcers, particularly around the ankles.
Sudden swelling or redness may indicate a blood clot, which requires immediate medical attention. Recognizing these warning signs early can prevent life-threatening complications and improve long-term outcomes.
Seek immediate medical care if you notice:
- Severe or worsening leg pain.
- Sudden swelling in one leg.
- Skin ulcers or open sores near the ankle.
- Redness, warmth, or tenderness along a vein.
- Bleeding from a varicose vein.
- Skin discoloration or hardening around the affected area.
Additional Clinical Indicators & Patient Awareness
Understanding symptom variations across different stages and populations helps in better diagnosis and timely treatment. Patients often overlook subtle symptoms until they become more severe, which can delay intervention.
Here you can watch the following to get better awareness in your daily life with varicose veins symptoms-
Signs of Varicose Veins in Daily Life
Beyond clinical observation, the signs of varicose veins can also appear during routine activities. Patients may notice visible vein bulging after standing for long hours or increased prominence after physical exertion. These signs often fluctuate throughout the day depending on circulation and posture.
Varicose Veins Symptoms in Legs During Activity
The varicose veins symptoms in legs tend to intensify with prolonged standing, walking, or sitting. Many individuals report a dull ache or heaviness that worsens by evening and improves with rest or leg elevation. This pattern is a key diagnostic clue in clinical evaluation.
Early Signs of Varicose Veins Often Ignored
The early signs of varicose veins are frequently subtle and dismissed as fatigue or muscle strain. However, recurring leg discomfort, mild swelling, or visible vein patterns should not be ignored, as they may indicate the beginning of venous insufficiency.
Varicose Veins Symptoms Female – Lifestyle Impact
The varicose veins symptoms female patients experience can also be influenced by lifestyle factors such as prolonged standing (e.g., teaching, nursing) or wearing high heels. Hormonal shifts combined with daily habits can accelerate symptom progression.
Comprehensive Care & Interventional Solutions for Varicose Veins
For individuals experiencing persistent discomfort, progressive vein enlargement, or complications associated with venous insufficiency, timely medical intervention is critical. Contemporary vascular medicine offers a spectrum of evidence-based, minimally invasive procedures such as endovenous ablation, sclerotherapy, and ultrasound-guided interventions designed to address the underlying hemodynamic dysfunction rather than just surface-level symptoms.
If you are considering clinical care, this in-depth resource on Varicose Vein Treatment provides a detailed overview of advanced therapeutic options, patient-centered treatment planning, and expected outcomes. It serves as a valuable guide for understanding how modern interventions can alleviate symptoms, prevent disease progression, and restore optimal vascular health.
Conclusion
Varicose veins are more than a cosmetic concern-they reflect underlying vascular dysfunction that can progressively worsen without proper care. Recognizing symptoms early allows for timely intervention, reducing the risk of complications such as ulcers or thrombosis.
A proactive approach that includes lifestyle modifications, medical evaluation, and appropriate treatment can significantly improve both vascular health and overall quality of life.
References
- Mayo Clinic Staff. (2024). Varicose veins: Symptoms and causes. Mayo Clinic.
- National Heart, Lung, and Blood Institute. (2023). Varicose veins. NIH.
- Medical News Today. (2024). Varicose veins: Causes, symptoms, and treatment.
- National Clinical Guideline Centre. (2013). Varicose veins in the legs. NICE Guidelines.
- StatPearls Publishing. (2023). Varicose Veins Epidemiology and Pathophysiology.
- (2022). Clinical presentation and pathophysiology of varicose veins.