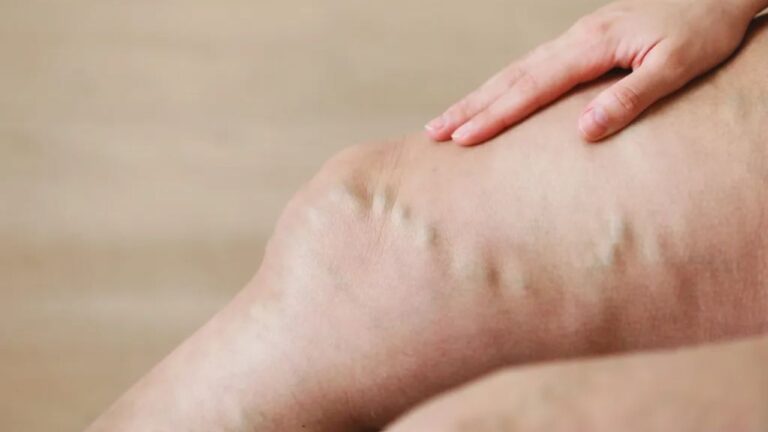
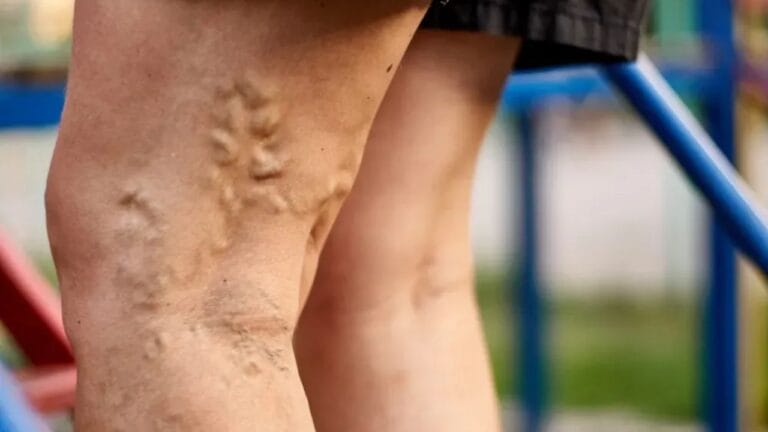
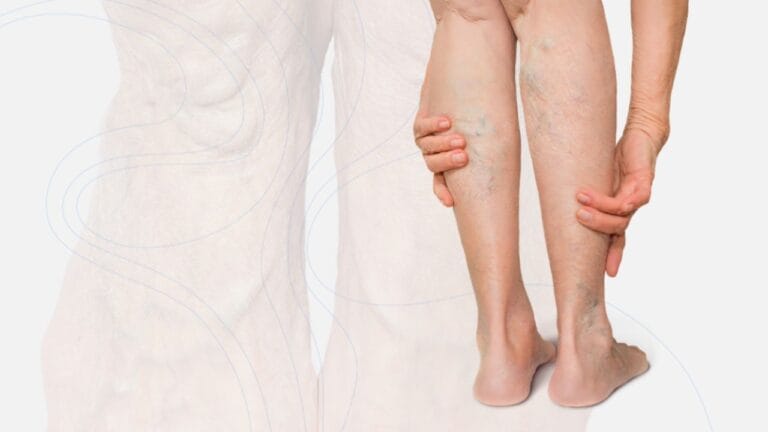
The actions that most worsen the symptoms of venous insufficiency are prolonged standing or sitting, wearing tight clothing, lack of physical activity, obesity, heat exposure, and smoking. These habits increase pressure in the leg veins, slow blood flow, and make symptoms like swelling, heaviness, varicose veins, and skin changes worse.
“Chronic venous insufficiency is heavily influenced by lifestyle. Small changes like moving regularly, maintaining a healthy weight, and avoiding long periods of standing can significantly reduce symptom progression and improve quality of life.”
– Vascular Specialist (based on clinical guidelines)
Understanding these aggravating actions is essential for managing venous insufficiency effectively and preventing complications.
Let’s take a closer look at the habits and daily actions that can make symptoms worse.
Which action would aggravate the clinical manifestations of venous insufficiency?
Certain everyday habits and lifestyle choices can significantly worsen the symptoms of venous insufficiency by increasing pressure in the leg veins and impairing proper blood flow. These actions may not seem harmful initially, but over time, they can contribute to increased swelling, discomfort, and progression of the condition. Recognizing and modifying these aggravating factors is a key step in managing symptoms effectively and improving overall vascular health.
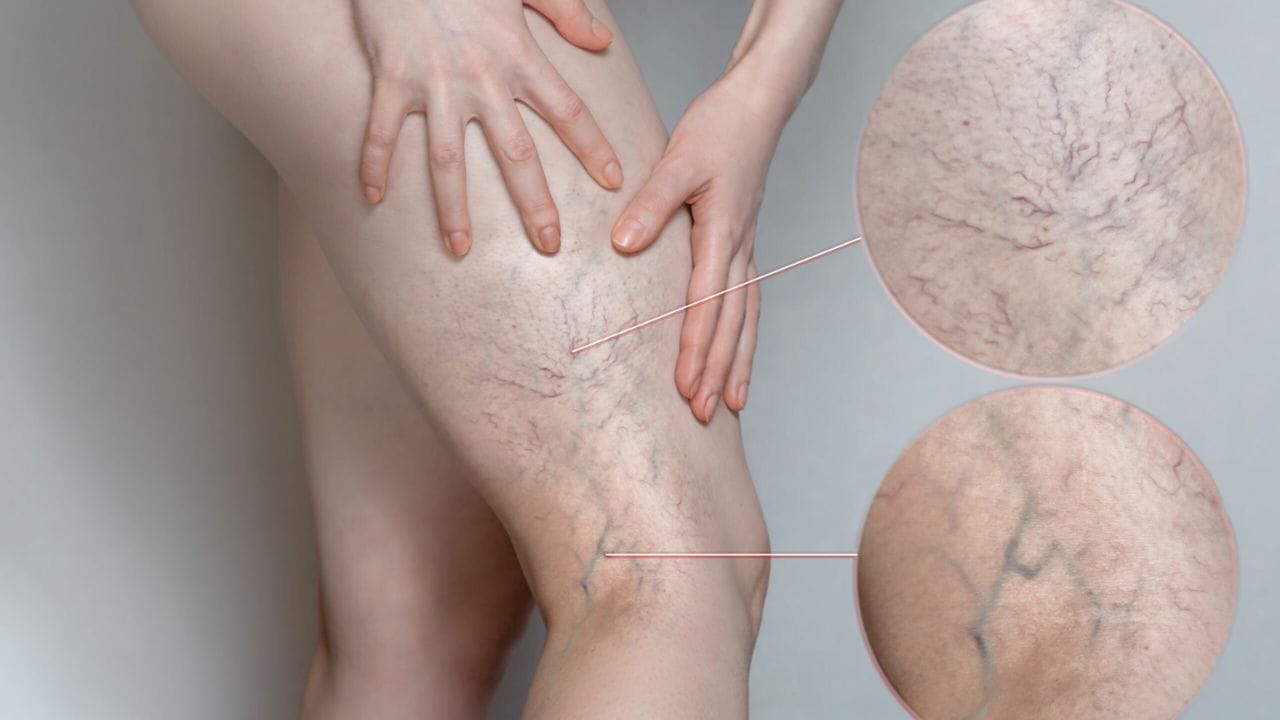
Key Facts About Venous Insufficiency
| Factors | Impact on Venous Insufficiency |
| Prevalence | Affects up to 20-40% of adults worldwide. |
| Prolonged standing jobs | Increases risk by 2-3 times. |
| Obesity | Significantly raises venous pressure and symptom severity. |
| Physical inactivity | Slows venous return and worsens pooling. |
| Compression therapy | Can reduce symptoms by up to 70% in mild-to-moderate cases. |
1. Prolonged Standing or Sitting
Remaining in a static position for long periods increases pressure in the leg veins. Gravity pulls blood downward, stretching vein walls and impairing valve function. Over time, this can worsen swelling, aching, and fatigue in the legs.
- Occupations involving long hours of standing or sitting, such as teaching, retail, or office work, are particularly risky.
- Frequent movement, stretching, or short walks can help maintain blood flow and reduce symptoms.
Aggravating Factors:
- Standing for more than 2-3 hours without movement.
- Sitting for extended periods without leg movement.
2. Wearing Tight or Restrictive Clothing
Clothing that compresses the waist, thighs, or calves can restrict venous blood flow. Tight pants, skinny jeans, or non-medical elastic garments may impair valve function, increase swelling, and worsen varicose veins.
- High heels limit the calf muscle pump, reducing blood return.
- Compression stockings are an exception as they are designed to improve venous circulation.
Aggravating Factors:
- Tight clothing around the legs or waist.
- Frequent wearing of high heels.
3. Lack of Physical Activity
The calf muscles act as a “secondary pump” to assist blood flow back to the heart. Sedentary behavior or inactivity weakens this mechanism, leading to blood pooling and increased venous pressure.
- Bed rest, prolonged travel, or a sedentary office lifestyle can aggravate venous symptoms.
- Regular walking or calf exercises help improve circulation.
Aggravating Factors:
- Sedentary lifestyle with minimal leg movement.
- Extended periods of immobility during travel.
4. Obesity and Excess Weight
Excess body weight increases pressure on leg veins, compressing tissues and straining vein walls. This contributes to swelling, skin changes, and varicose vein formation.
- Abdominal obesity increases intra-abdominal pressure, further impairing venous return.
- Maintaining a healthy weight can reduce venous strain and improve symptoms.
Aggravating Factors:
- Rapid or sustained weight gain.
- Excess abdominal fat.
5. Exposure to Heat
Heat causes veins to dilate, which can worsen blood pooling in the legs. Hot baths, saunas, or direct sun exposure may increase swelling, heaviness, and discomfort.
This also explains why does venous insufficiency cause edema is a common concern, as heat can significantly intensify fluid accumulation in the lower limbs. However, symptoms often worsen during the summer months or after prolonged sun exposure. Cool environments and leg elevation can provide temporary relief.
Aggravating Factors:
- Hot baths, saunas, or sunbathing
- Wearing insulating clothing in hot weather
6. Smoking and Poor Lifestyle Habits
Smoking damages blood vessels, reduces vascular elasticity, and impairs circulation. Combined with sedentary habits, smoking accelerates vein valve deterioration and increases the risk of blood clots. Excess alcohol consumption can worsen edema and inflammation.
A healthy lifestyle supports vein function and reduces complications. It is also important to understand long-term management strategies, especially when considering whether can venous insufficiency be reversed through lifestyle changes and medical care.
Aggravating Factors:
- Smoking and tobacco use.
- Excessive alcohol intake.
- Lack of regular exercise or poor nutrition.
Helpful vs Harmful Habits For Venous Insufficiency:
| Helpful Habits | Harmful Habits |
| Walking regularly | Sitting or standing for long hours |
| Wearing compression stockings | Wearing tight clothing |
| Maintaining a healthy weight | Obesity |
| Elevating legs | Prolonged heat exposure |
| Staying active | Smoking |
Clinical Insight For Venous Insufficiency:
Venous insufficiency is a progressive condition if left unmanaged. Early lifestyle modifications combined with compression therapy can significantly reduce symptom severity and delay complications such as venous ulcers and skin thickening.
Epidemiological data show that venous insufficiency affects approximately 20–30% of adults globally, with prevalence increasing significantly with age.
Clinical studies indicate that up to 60% of patients experience leg edema, while nearly 15% may develop venous ulcers in advanced stages if not properly managed.
Compression therapy, a cornerstone of treatment, has demonstrated strong effectiveness, with healing rates ranging from 40% to over 95% in venous ulcers, depending on adherence and treatment quality.
In addition, consistent use of compression stockings can reduce ulcer recurrence rates dramatically (as low as 4% with adherence vs. up to 79% without), highlighting the importance of long-term management.
Overall, evidence shows that early intervention not only improves symptoms but also reduces the risk of complications such as chronic ulcers, recurrent disease, and long-term tissue damage.
When to Seek Medical Attention for Venous Insufficiency
Venous insufficiency often starts with mild symptoms like leg heaviness, swelling, or occasional cramps. However, it’s crucial to recognize when these signs indicate a more serious problem that requires medical evaluation. Prompt attention can prevent complications such as chronic pain, skin changes, or even blood clots.
You should consider seeking medical attention if you notice any of the following:
- Sudden swelling, redness, or warmth in the leg: This could be a sign of a blood clot (deep vein thrombosis), which requires immediate medical care.
- Persistent or worsening leg pain and cramping: Continuous discomfort, especially after rest or at night, may indicate progressive venous disease.
- Non-healing ulcers, sores, or skin changes: Open wounds or darkened, thickened skin on the legs are warning signs of chronic venous insufficiency and need professional evaluation.
For a thorough assessment and personalized treatment options, consulting a specialist is highly recommended. Dr. Rema Malik is an experienced physician in vascular health who can evaluate symptoms, recommend diagnostic tests, and guide patients on the most effective therapies for venous insufficiency.
- Rapid progression of varicose veins or visible skin changes: If new varicose veins appear quickly, or if the skin becomes discolored, hardened, or itchy, it’s time to seek professional care.
- Severe or persistent leg heaviness, fatigue, or swelling: These can affect daily life and may worsen without intervention, making early medical consultation essential.
Early evaluation not only helps in symptom management but also reduces the risk of serious complications such as chronic venous ulcers, infections, and long-term vascular damage. Seeking medical guidance ensures that treatment ranging from lifestyle modifications and compression therapy to minimally invasive procedures is tailored to the severity of your condition.
Final Note
Taking control of your venous health starts with awareness and action. Simple lifestyle changes like staying active, managing weight, and using compression therapy can make a world of difference in preventing complications and improving your quality of life. Don’t wait for symptoms to worsen; early attention can keep your legs healthy, comfortable, and strong.
If you notice persistent swelling, heaviness, or skin changes, consult a vascular specialist today to get personalized guidance and treatment. Your veins and your future self will thank you!
Here’s to healthier legs and a more active, vibrant life!
FAQs
Can venous insufficiency be cured?
While vein damage cannot always be reversed, lifestyle changes, compression therapy, and medical treatments like sclerotherapy or minimally invasive vein surgery can manage symptoms and prevent progression.
Are compression stockings effective?
Yes, medical-grade compression stockings help improve blood flow, reduce swelling, and alleviate discomfort. They are safe and effective for most patients.
How does exercise help with venous insufficiency?
Exercise, especially walking, calf raises, and ankle flexions, strengthens leg muscles, enhances the calf pump, and improves venous return, reducing symptoms like swelling and heaviness.
Is heat always harmful?
While prolonged heat exposure can worsen symptoms, brief exposure or warm showers are usually safe. Cooling the legs or elevating them afterward helps mitigate negative effects.